News and Views - Imaging in Medicine (2010) Volume 2, Issue 3
News & Views in ... Imaging in Medicine 2:3
Abstract
CT scans aid early detection of emphysema
A team at the University of Iowa (IA, USA) has recently published their findings on the possibility of using CT scans to identify smokers at an increased risk of emphysema.
Their study, published in the Proceedings of the National Academy of Science, aimed to investigate the early regional vascular dysfunction that was hypothesized to precede smoking-associated emphysema.
Pulmonary emphysema is a form of chronic obstructive pulmonary disease in which the alveoli of the lung become abnormally inflated and consequently damaged, making it harder for sufferers to expel carbon dioxide. Smokers have an increased risk of developing emphysema, which is currently an incurable and chronic disease.
Using multidetector-row CT perfusion imaging the team monitored the blood-flow patterns in the lungs of a group of 24 smokers and 17 nonsmokers, both of which demonstrated normal spirometry. They found that 12 of the smokers had slight evidence of emphysema and also demonstrated the most disrupted patterns of blood flow compared with the other participants.
Leader of the research group Eric Hoffman comments on the teams findings, “Although the underlying causes of emphysema are not well understood, smoking increases the risk of developing the disease. Our study suggests that some smokers have an abnormal response to inflammation in their lungs; instead of sending more blood to the inflamed areas to help repair the damage, blood flow is turned off and the inflamed areas deteriorate”.
The group believes that this tool can detect the occurrence of early emphysema- related changes in susceptible smokers. They also note that it may prove useful in other respiratory diseases, as noted by Hoffman, “Our discovery may also help researchers understand the underlying causes of this disease and help distinguish this type of emphysema from other forms of chronic obstructive pulmonary disease. This type of CT scan could even be a tool to test the effectiveness of new therapies by looking at the changes in lung blood flow.”
Source: Alford SK, van Beek EJ, McLennan G, Hoffman EA: Heterogeneity of pulmonary perfusion as a mechanistic image-based phenotype in emphysema susceptible smokers. Proc. Natl Acad. Sci. USA 107(16), 7485–7490 (2010).
CT scan radiation dose could be exposed by automatic tracking device
A collaboration of researchers from the USA has reported on a system that collates information on radiation dose received by patients undergoing CT examinations.
Scientists have presented their research on a radiation dose tracking system at the American Roentgen Ray Society 2010 Annual Meeting (San Diego, CA, USA, 2–7 May 2010). The computer-based system automatically tracks patient-specific radiation dose exposure from CT scans. A total of 518 dose reports were randomly selected for the study, and the authors report that the system, dubbed Valkyrie, was accurate in extracting dose information in 100% of these scans. Approximately 50% of radiation dose exposure administered in medical care comes from CT examinations. George Shih, lead author of the study comments, “The purpose of the computer-based system, called Valkyrie, is to extract the radiation dose information from CT dose reports so as to eventually perform automated quality control, promote radiation safety awareness, and provide a longitudinal record of patient health care-related radiation exposure.”
The dose exposure takes into account the patient’s size and weight and, if used at every CT examination, provides a method for patients to track their cumulative dose of radiation exposure. Shih continues, “Valkyrie will eventually enable patients to keep a digital log of their healthcare-related radiation dose. While the system is functional, it is still in a development phase. We hope that eventually all hospitals will use Valkyrie or something equivalent for all CT studies, so that we can provide more accurate healthcare-related radiation- dose information to our patients’ personal health records.” Scientists from Columbia University Medical Center (New York, NY, USA), Cornell University (Ithaca, NY, USA) and the University of Kentucky (Lexington, KY, USA) were involved in the study.
Source: Shih G, Lu Z, Kennedy D et al.: Valkyrie: automated framework for digital radiation dose reporting from CT dose reports. Presented at: American Roentgen Ray Society 2010 Annual Meeting. San Diego, CA, USA, 2–7 May 2010.
US university receives multimillion award for MRI study of muscular dystrophy
The University of Florida (FL, USA) has been awarded US$7.5 million by the NIH to study the use of MRI in determining the natural progression of the disease.
Duchenne muscular dystrophy affects approximately one in 4000 boys each year in the USA. The muscles of individuals with the disease progressively weaken and lose the ability to regenerate after injury. Many patients require a wheelchair by the time they reach 12 years of age. The disease eventually affects the heart and respiratory system, leading to fatal cardiorespiratory failure in their 20s.
Krista Vandenborne, an Associate Dean for Research and Planning at the University of Florida College of Public Health and Health Professions and Chair of the Department of Physical Therapy comments, “The lack of a reliable assessment tool for measuring muscle function in patients with Duchenne inhibits the transfer of new therapies from the lab to clinical trials. MRI allows you to look at the structure of a muscle tissue in a very objective way with a large amount of detail. Our goal is to develop MRI as a tool to see the progression of the disease, but more importantly, to determine if a new treatment is effective or not, giving researchers rapid feedback about potential new drugs.”
The funding will support researchers at Oregon Health and Science University (OR, USA), Children’s Hospital of Philadelphia (PA, USA) and the University of Pennsylvania (PA, USA). Researchers at the four sites will conduct MRI measurements of muscle in 100 boys with Duchenne, aged 5–14 years, over a 5-year period.
“We are confident that by the end of the study we will be able to provide clear guidelines for how MRIs should be performed in Duchenne muscular dystrophy and that MRIs will be a valuable tool in clinical trials and drug tests targeting potential Duchenne treatments”, Vandenborne said.
Source: University of Florida Office of News & Communications: http://news.health.ufl. edu/2010
Fatal heart problem diagnosed by PET/CT
Scientists in Germany use latest molecular imaging techniques to distinguish between the acute and chronic form of aortic dissection.
Scientists investigating aortic dissection have used imaging in a recent study published in the Journal of Nuclear Medicine. Aortic dissection is a tear in the aorta, which has serious hemorrhaging consequences. The tear begins in the tunica intima, causing blood to flow into the tunica media and therefore laminal tearing along this medial layer.
Acute cases cause severe pain and the location of the pain corresponds to the location of the dissection. In cases where no pain occurs for 2 weeks following onset, the aortic dissection is chronic. Hans-Henning Eckstein, a Professor at the Technical University of Munich in Germany and corresponding author explains the importance of the study, “It is critical to patients’ survival that doctors are able to verify acute or exclude chronic aortic dissection so they can decide the best course of treatment – whether that means rushing the patient to surgery in some cases or using b-blockers to lower the blood pressure”.
Conventional imaging modalities do not discriminate between the acute and chronic forms, therefore researchers from Technical University of Munich have investigated the possibility of using 18F-FDG PET/CT for this purpose. They proposed that acute aortic dissection would have evidence of reparatory hypermetabolism in the lacerated wall. Conversely, in the case of chronic disease, the scarred aortic tissue would have a low concentration of metabolites. Results of the study showed that 18F-FDG uptake at the injured aortic wall or dissection membrane was significantly higher in acute aortic dissection than in chronic stable aortic dissection. A total of 18 patients took part in the study; there were nine acute cases, two with symptomatic progressive aortic dissection and seven known to have the chronic stable form. All participants in the study underwent 18F-FDG PET/CT. Images were analyzed qualitatively and quantitatively considering 18F-FDG uptake patterns and the standardized uptake values of the aortic wall, dissection membrane, and luminal 18F-FDG activity.
The authors conclude that, “Our results indicate that 18F-FDG PET/CT might be useful in differentiation of acute from chronic AD in clinically unclear cases. However, larger studies are needed to confirm our preliminary results”.
Source: Reeps C, Pelisek J, Bundschuh RA et al.: Imaging of acute and chronic aortic dissection by 18F-FDG PET/CT. J. Nucl. Med. 51(5), 686–691 (2010).
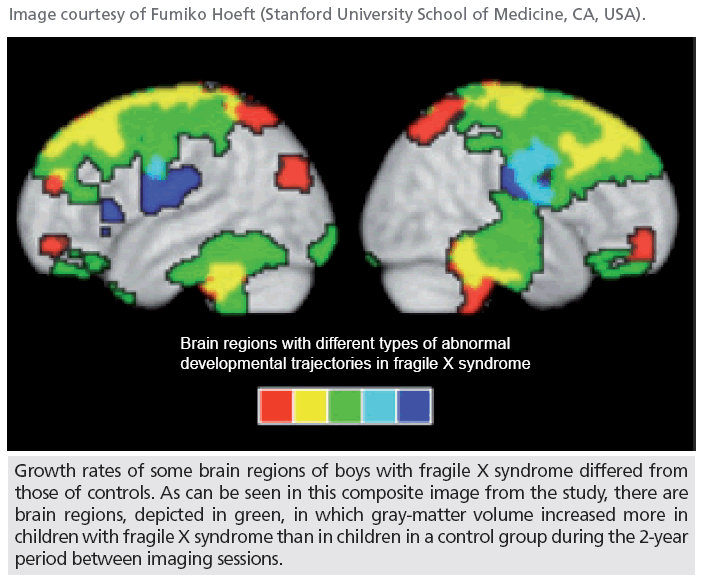
Longitudinal neuroimaging in fragile X syndrome research
Recent research carried out by scientists in the USA has revealed differences between the brains of boys with fragile X syndrome (FXS) and boys without the syndrome. FXS is the most common cause of inherited intellectual disability and autism, affecting one in 4000 people. The disease is triggered by a mutation in a gene on the X chromosome. High-resolution MRI was used to investigate FXS in boys, with the results of the study providing hope for better detection and treatment of the disease.
The study was a collaboration between researchers from the Stanford University School of Medicine (CA, USA) and from the University of North Carolina, Chapel Hill (NC, USA). The authors conclude that their results indicate that white matter abnormalities are not caused by “secondary connectional dysregulation between morphologically atypical brain structures”. Instead, the authors surmise that the abnormalities are related to axonal pathology triggered by primary fragile X mental retardation 1 protein deficiency.
The noninvasive imaging technique used in the research enables the study of specific genetic factors on neurodevelopment in the living human brain. A total of 41 boys with FXS, aged between 1 and 3 years, took part in the study; their brains were examined and followed-up 2 years later. Findings from these boys were compared with developmentally matched controls (n = 28). The authors describe their results, “We found enlarged GMV in the caudate, thalamus, and fusiform gyri and reduced GMV in the cerebellar vermis in FXS at both timepoints, suggesting early, possibly prenatal, genetically mediated alterations in neurodevelopment.”
Source: Hoeft F, Carter JC, Lightbody AA, Cody Hazlett H, Piven J, Reiss AL: Region-specific alterations in brain development in one- to three-year-old boys with fragile X syndrome. Proc. Natl Acad. Sci. USA (2010) (Epub ahead of print).