News and Views - Imaging in Medicine (2010) Volume 2, Issue 1
News & Views in ... Imaging in Medicine 2:1
Abstract
Obesity and elevated heart rates associated with coronary artery MDCT of reduced quality
German researchers have conducted a large, multicenter trial to investigate the impact of patient characteristics on the diagnostic accuracy of multidetector CT (MDCT) for the detection of coronary artery stenosis. The results indicate that increasing BMI, increasing heart rate and the presence of breathing artifacts are associated with poorer image quality.
Many patients with suspected coronary artery disease have undergone MDCT scans owing to its diagnostic accuracy and reliability, however, this is dependent on image quality. Therefore, this international study was conducted to determine what affects the image quality of MDCT scans. Invasive coronary angiography is the conventional technique employed for suspected coronary artery disease.
“…results indicate that increasing BMI, increasing heart rate and the presence of breathing artifacts are associated with poorer image quality.”
To be eligible for the study, participants needed to have a coronary artery calcification (CAC) score of 600 Agatston units or less. The CAC score is determined by a cardiac CT scan and is a noninvasive way of determining the presence, location and extent of calcified plaque in the coronary arteries. A total of 291 patients took part (214 men and 77 women) and the mean age was 59.3 years.
Each MDCT scan was given an image quality score that ranked it among the other MDCT scans.
Quantitative coronary angiography was used to assess the accuracy of quantitative MDCT to detect significant stenoses in each patient and for each vessel using a modified 19‑segment model. A number of factors were measured to determine whether they had an effect on image quality and accuracy, achieved through multiple logistic regression. The factors taken into account were CAC, obesity, gender, heart rate and heart rate variability. Diagnostic analysis was determined for image quality strata using receiver operating characteristic curves.
“Many patients with suspected coronary artery disease have undergone MDCT scans owing to its diagnostic accuracy and reliability, however, this is dependent on image quality.”
The study gave rise to interesting results. Some factors were found to be associated with poorer image quality including: increasing BMI (odds ratio [OR] = 0.89; p < 0.001), increasing heart rate (OR = 0.90; p < 0.001) and the presence of breathing artifact (OR = 4.97; p < 0.001). However, gender, CAC score and heart rate variability were not.
There were some other f indings, although not as statistically significant as those listed above: examinations of black patients showed that they had significantly poorer image quality that those of white patients (OR = 0.58; p = 0.04). The authors also concluded that, “At a vessel level, CAC score and age were associated with reduced diagnostic accuracy.”
Source: Dewey M, Vavere AL, Arbab-Zadeh A et al.: Patient characteristics as predictors of image quality and diagnostic accuracy of MDCT compared with conventional coronary angiography for detecting coronary artery stenoses: CORE‑64 Multicenter International Trial. AJR Am. J. Roentgenol. 194(1), 93–102 (2010).
New mammography screening recommendations
The Society of Breast Imaging (SBI) and the American College of Radiology (ACR) have issued new guidelines regarding mammography screening for breast cancer
“In addition to starting screening at 40 years of age, the guidelines also recommend that screening should start earlier in high-risk patients.”
Breast cancer screening should begin at 40 years. This guideline is from new recommendations from the SBI and the Breast Imaging Commission of the ACR. The recommendations are aimed at patients and clinicians to advise them on the use of imaging to screen for breast cancer.
Mammography is currently the standard technique for breast cancer screening, and it has been demonstrated to reduce deaths from the disease. However, mammography is not without its limitations, and other techniques have been implemented in particular cases recently. Tools such as ultrasound and MRI may be more appropriate in some cases, for example, in women who may be at increased risk for developing breast cancer.
Lead author Carol Lee, from Memorial Sloan-Kettering Cancer Center (New York, NY, USA) said, “The significant decrease in breast cancer mortality, which amounts to nearly 30% since 1990, is a major medical success and is due largely to earlier detection of breast cancer through mammography screening. For women with the highest risk of developing breast cancer, screening technologies in addition to mammography have been adopted.”
In addition to starting screening at 40 years of age, the guidelines also recommend that screening should start earlier in high-risk patients. In high-risk patients, annual breast cancer screening should begin by 30 years of age, but not before age 25 years of age.
Published in the January 2010 issue of the Journal of the American College of Radiology, the recommendations are based on available evidence. Where evidence is unavailable, opinions of the fellows and executive committee of the SBI and members of the Breast Imaging Commission of the ACR have formed the basis of the report.
“Evidence to support the recommendation for regular periodic screening mammography comes from the results of several randomized trials (RCTs) conducted in Europe and North America that included a total of nearly 500,000 women. Overall, based on a meta-analysis of the RCTs, there was a 26% reduction in mortality,” said Lee.
Source: Lee CH, Dershaw DD, Kopans D et al.: Breast cancer screening with imaging: recommendations from the society of breast imaging and the ACR on the use of mammography, breast MRI, breast ultrasound and other technologies for the detection of clinically occult breast cancer. J. Am. Coll. Radiol. 7(1), 18–27 (2010).
Identifying malignant breast cancer without an invasive biopsy
Scientists from the Kimmel Cancer Center at Jefferson (PA, USA) may have discovered a way to spot malignant breast tumors without a biopsy
Mathew Thakur, Professor of Radiology at Jefferson Medical College of Thomas Jefferson University and Director of Radiopharmaceutical Research and Nuclear Medicine Research, and his colleagues, have been working on an agent called 64Cu‑TP3805, which can be used to assess tumors via PET imaging. The agent is able to identify a tumor by seeking out VPAC1, a biomarker that is overexpressed in developing tumors.
“The challenge has been to develop an imaging agent that will target a specific, fingerprint biomarker that visualizes malignant breast lesions early and reliably,” remarked Thakur.
Existing imaging methods miss up to 30% of breast cancers and are currently unable to discriminate malignant from benign tumors. This is why patients require invasive biopsies. These biopsies can cause considerable stress for patients and have significantly high costs. For these reasons there is a need for alternative procedures, especially given that 5.6 million biopsies performed discover only benign lesions.
The scientists used MMTVneu mice, which are able to develop breast tumors spontaneously, to compare images using 64Cu‑TP3805 with images using the ‘goldstandard’ agent, 18F‑FDG. A total of ten tumors were found on the mice; four of which were detected by both imaging agents and a further four of which were detected by 64Cu‑TP3805 alone. These eight tumors all overexpressed VPAC1 and were found to be malignant by histology. The remaining tumors were benign and were only detected with 18F‑FDG. The new agent failed to detect them as they did not express VPAC1.
Thakur believes that, “If this ability of 64Cu‑TP3805 holds up in humans, then in the future, PET scans with 64Cu‑TP3805 will signif icantly contribute to the management of breast cancer.”
Source: Thakur ML, Devadhas D, Zhang K et al.: Imaging spontaneous MMTVneu transgenic murine mammary tumors: targeting metabolic activity versus genetic products. J. Nucl. Med. 51(1), 106–111 (2009).
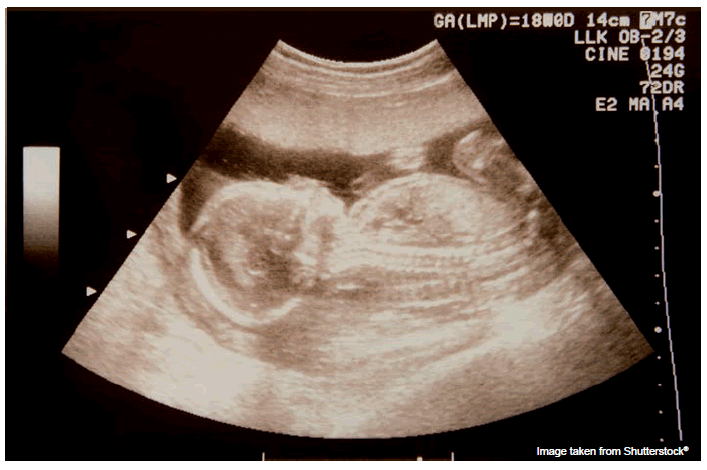
Canadian study reports increase in number of pregnancy ultrasounds
Scientists from institutes in Hamilton and Toronto, ON, Canada have conducted a large population-based study to investigate the use of prenatal ultrasonography in Ontario, Canada. They found that the number of ultrasound scans performed during the study had increased by 55%, even in low-risk pregnancies.
Although the risk involved by increasing the number of ultrasound scans during pregnancy is not currently known, the investigators were interested to know whether the last decade has seen an increase in the number of ultrasound scans.
Commencing in 1996, the investigators evaluated the relative risk (RR) for the change in rates of ultrasonography for each subsequent year. The RR was adjusted for maternal age, income, rural residence, maternal comorbidities, receipt of genetics consultation or amniocentesis and history of complications in a prior pregnancy.
A total of 1,399,389 singleton deliveries were enrolled on the study, which finished in 2006. The rate of prenatal ultrasonography increased from 2055 per 1000 pregnancies in 1996 to 3264 per 1000 in 2006 (adjusted RR: 1.55; 95% CI: 1.54–1.55). The increase was similar between women with low-risk pregnancies and those with high-risk pregnancies. Also to be considered is the finding that the increase in the number of ultrasounds was more pronounced among low-risk pregnancies than among high- risk pregnancies.
The study showed that the proportion of pregnancies with at least four ultrasound examinations in the second or third trimesters increased from 6.4 to 18.7% (adjusted RR: 2.68; 95% CI: 2.61–2.74) during the 10‑year study. “Our findings are consistent with a growing body of evidence suggesting that some health interventions most beneficial to high-risk individuals are frequently directed at apparently lowrisk populations,” writes lead author John You, McMaster University (Hamilton, ON, Canada). “While the benefits of prenatal ultrasound in high-risk pregnancies may be more clear, the value of repeat ultrasounds in low-risk patients is not.”
Considering that the current recommended number of ultrasound examinations for an uncomplicated pregnancy is two, the findings may call for further discussion among medical experts. The authors conclude in their that abstract, “Efforts to promote more appropriate use of prenatal ultrasonography for singleton pregnancies appear warranted.”
Source: You JJ, Alter DA, Stukel TA et al.: Proliferation of prenatal ultrasonography. CMAJ (2010) (Epub ahead of print).