Editorial - Research on Chronic Diseases (2018) Volume 2, Issue 1
Genomic medicine and acute cardiovascular disease progression in diabetes
- *Corresponding Author:
- Ian James Martins
Centre of Excellence in Alzheimer’s Disease Research and Care
Sarich Neuroscience Research Institute
Edith Cowan University Verdun Street, Nedlands, 6009
Western Australia, Australia
E-mail: i.martins@ecu.edu.au
Abstract
Keywords
genomic medicine, acute cardiovascular disease, immune system, Sirtuin 1, heat shock protein, nutritional therapy, mitophagy, NAFLD, diabetes
Editorial
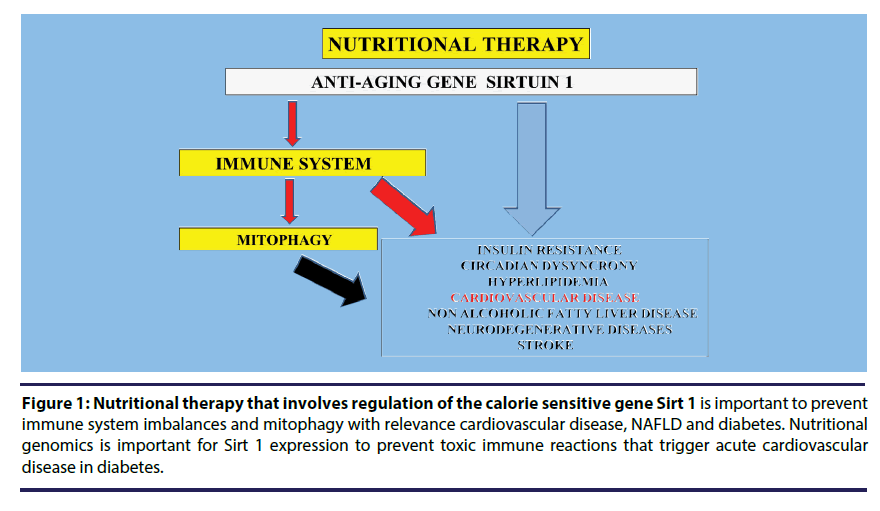
Health promotion and prevention of disease has now become of major interest to the scientific and medical community with genomic medicine now important to modern medicine [1]. Nutritional genomics [2] allows the use of nutrition research to determine nutritional interventions that enables gene expression that improves the health and wellbeing of individuals in the community. The future of science and medicine in disease progression in diabetes is now dependent on nutritional genomics that involve the anti-aging genes [3] that are essential to prevent insulin resistance, circadian dysynchrony, hyperlipidemia, acute cardiovascular disease, nonalcoholic fatty liver disease (NAFLD) and neurodegenerative diseases. The anti-aging gene Sirtuin 1 (Sirt 1) is now important to the prevention of chronic disease [4-6] with its critical involvement in the immune system that involves toxic immune reactions [7-9] connected to the acceleration of various organ diseases (Figure 1) with relevance to disease progression in diabetes in various communities [10,11].
Figure 1: Nutritional therapy that involves regulation of the calorie sensitive gene Sirt 1 is important to prevent immune system imbalances and mitophagy with relevance cardiovascular disease, NAFLD and diabetes. Nutritional genomics is important for Sirt 1 expression to prevent toxic immune reactions that trigger acute cardiovascular disease in diabetes.
Sirt 1 defects in diabetes now provide Sirt 1 as a gene associated with multi-organ gene regulatory influences [12] with molecular targets relevant to the development of immune dysfunction, organ diseases and the metabolic syndrome. Sirt 1 is nicotinamide adenine dinucleotide (NAD+) dependent class III histone deacetylase (HDAC) and its regulation of the immune system is critical to the prevention of mitophagy with connections of Sirt 1 that target transcription factors such as p53 to adapt gene expression to the immune system, metabolic activity with deacetylation of nuclear receptors associated with insulin resistance [5]. Sirt 1 expression can be altered by micro RNA (mi-34a, mi-132 and mi-122) that determine p53 effects on Sirt 1 expression with relevance to insulin resistance, cardiovascular disease and metabolic disease [5].
The causes of the global burden of cardiovascular disease has become of major concern to various regions in the world [13]. Nutrition and genomic medicine in diabetes are essential to maintain insulin therapy and of crucial importance to cardiovascular disease and to the prevention of toxic immune reactions [14,15]. Sirt 1 repression with uncontrolled toxic immune reactions [7- 9] and mitophagy should now be included in immune mediated inflammatory cardiovascular diseases [16,17] with relevance to the trigger of cardiovascular disease progression in diabetes (Figure 1). Multi-organ disease now involves Sirt 1 repression and mitophagy [5,6,18,19] connected to climate and pollution alterations that trigger acute myocardial infarction or cardiac arrhythmias [20-22]. Sirt 1 repression is related to defective heat shock protein 70 (HSP 70) metabolism with Sirt 1 now referred to as the heat shock gene [23,24]. HSP 70 is important to mitochondrial apoptosis and autoimmune disease [25,26] with elevated HSPs in man connected to cardiovascular disease [27,28]. Heat therapy in diabetics [29] should be carefully controlled with core brain temperature alterations that may lead to complete inactivation of nutritional Sirt 1 genomics with relevance to immune reactions, acute cardiovascular disease and NAFLD.
Nutritional interventions [30] to activate Sirt 1 are essential in the treatment of insulin resistance and the prevention of multiple organ disease in diabetes [31]. The involvement of nutrition and the immune system has become important to nutritional genomics with mitophagy in neurons of critical concern to maintain neuron lifespan relevant to global cardiovascular disease, chronic metabolic and neurodegenerative diseases [32]. Sirt 1 inhibitors such as bacterial lipopolysaccharides have become relevant to disease progression in diabetes [33] with Sirt 1 repression associated with autoimmunity, NAFLD and insulin resistance [34]. Nutritional genomics with relevance to science and medicine requires the assessment of caffeine as a trigger for acute cardiovascular disease [35]. Caffeine is a Sirt 1 modulator [36] and its role in the induction of Type 3 diabetes is linked mitophagy and NAFLD [37,38]. Dietary fat (gm/day) intake determines caffeine metabolism [39] with relevance to the use of Sirt 1 activators [37,40] in genomic and nutritional medicine in the prevention of acute cardiovascular disease in diabetic.
Conclusion
Nutritional genomics and regulation of Sirt 1 has become important to the treatment of diabetes and the progression of various organ diseases. Sirt 1 inactivation by heat/cold stress interrupts HSPs metabolism connected to defective immunometabolism and mitophagy. Science and medicine and its relevance to genomic medicine needs to consider Sirt 1 gene expression with its relevance to diabetes and accelerated immune reactions that cause acute cardiovascular disease. Factors such as caffeine, body temperature and pollution need to be considered as the trigger for acute cardiovascular disease associated with the progression of NAFLD and diabetes.
Acknowledgements
This work was supported by grants from Edith Cowan University, the McCusker Alzheimer’s Research Foundation and the National Health and Medical Research Council.
References
- Elliott R, Ong TJ, Nutritional genomics Science medicine and the future. Bio Med J 32(4), 1438–1442 (2002).
- Kumar D. From evidence-based medicine to genomic medicine. Genomic Med. 1, 95–104 (2007).
- Martins IJ. Anti-Aging Genes Improve Appetite Regulation and Reverse Cell Senescence and Apoptosis in Global Populations. AAR 5, 9-26 (2016).
- Martins IJ. Genomic Medicine and Management of Genetic Disorders. J Genet. Disord. 1, 06 (2017).
- Martins IJ. Unhealthy Nutrigenomic Diets Accelerate NAFLD and Adiposity in Global communities. J Mol Genet Med 9, 1-11 (2015).
- Martins IJ. Induction of NAFLD with Increased Risk of Obesity and Chronic Diseases in Developed Countries. OJEMD. 4, 90-110 (2014).
- Martins IJ. Antimicrobial activity inactivation and toxic immune reactions induce Epilepsy in human. J Med Discov. 2, 1-7 (2017).
- Martins IJ. Appetite Control and Nutrigenomic Diets are Connected to Immune Regulation and Diabetes Prevention. EC. Nutrition. 12(3), 120-123 (2017).
- Martins IJ. Antibiotic Resistance Involves Antimicrobial Inactivation in Global Communities. SAJ. Pharma. Pharmacol. 2, 102 (2017).
- Martins IJ. Diet and Nutrition reverse Type 3 Diabetes and Accelerated Aging linked to Global chronic diseases. J Diab Res Ther. 2, 1-6 (2016).
- Martins IJ. Diabetes and Organ Dysfunction in the Developing and Developed. GJMR. 15, 15-21(2015).
- Anderson WD, DeCicco D, Schwaber JS. A data-driven modeling approach to identify disease-specific multi-organ networks driving physiological dysregulation. PLoS Comput Biol. 13, e1005627 (2017).
- Roth GA, Johnson C, Abajobir A. Global Regional and National Burden of Cardiovascular Diseases for 10 Causes 1990 to 2015. J Am Col Cardio.70, 1-25 (2017).
- Martins IJ. Insulin Therapy Inactivation is connected to NAFLD and Diabetes Severity Index. J Diab Clin Stud. 1, 01-03 (2017).
- Xiu F, Stanojcic M, Diao L. Stress Hyperglycemia Insulin Treatment and Innate Immune Cells. Int J Endocrinol. 1-9 (2014).
- Fernández Gutiérrez B, Perrotti PP, Gisbert JP. Cardiovascular disease in immune-mediated inflammatory diseases A cross-sectional analysis of 6 cohorts. Medicine Baltimore. 96: e7308 (2017).
- Frantz S, Bauersachs J, Kelly RA. Innate immunity and the heart. Curr Pharm Des. 11, 79-90 (2005).
- Vásquez Trincado C, García-Carvajal I, Pennanen C. Mitochondrial dynamics, mitophagy and cardiovascular disease. J Physiol. 509-525 (2016).
- Bravo San Pedro JM, Kroemer G, Galluzzi L. Autophagy and Mitophagy in Cardiovascular Disease. Circ Res. 120, 1812-1824 (2017).
- Tofler GH, Muller JE. Triggering of acute cardiovascular disease and potential preventive strategies. Circulation. 114, 1863-1872(2006).
- Link MS, Dockery DW. Air pollution and the triggering of cardiac arrhythmias. Curr Opin Cardiol. 25, 16-22 (2010).
- Claeys MJ, Rajagopalan S, Nawrot TS. Climate and environmental triggers of acute myocardial infarction. Eur Heart J. 38, 955-960 (2017).
- Martins IJ. Heat shock gene Sirtuin 1 regulates post-prandial lipid metabolism with relevance to nutrition and appetite regulation in diabetes Int J Diab Clin Diagn. 3, 20 (2016).
- Martins IJ. Type 3 diabetes with links to NAFLD and Other Chronic Diseases in the Western World. Int J Diab. 1, 1-5 (2016).
- Martins IJ. Regulation of Core Body Temperature and the Immune System Determines Species Longevity. Curr Updates. Gerontol. 1, 1-6 (2017).
- Martins IJ, Defective Interplay between Adipose Tissue and Immune System Induces Non Alcoholic Fatty Liver Disease. Updates. Nutr. Disorders. Ther. 1, 2-4 (2017).
- Madrigal Matute J, Martin-Ventura JL, Blanco Colio LM. Heat-shock proteins in cardiovascular disease. Adv Clin Chem. 54, 1-43 (2011).
- M. Zilaee, GA Ferns, M Ghayour Mobarhan. Heat shock proteins and cardiovascular disease. Adv Clin Chem. 64, 73-115 (2014).
- Martins IJ. Heat Therapy with Relevance to the Reversal of NAFLD and Diabetes. J Diabetes Metab Disord. 4, 01-8 (2017).
- Martins IJ. Overnutrition Determines LPS Regulation of Mycotoxin Induced Neurotoxicity in Neurodegenerative Diseases. Int J Mol Sci. 16, 29554–29573 (2015).
- Martins IJ. Single Gene Inactivation with Implications to Diabetes and Multiple Organ Dysfunction Syndrome. J Clin Epigenet. 3, 1-8 (2017).
- Martins IJ. Early diagnosis of neuron mitochondrial dysfunction may reverse global metabolic and neurodegenerative disease. GJMR. 2, 1-8 (2016).
- Martins IJ. The Future of Genomic Medicine Involves the Maintenance of Sirtuin 1 in Global Populations. Int J Mol Biol. 2, 13 (2017).
- Martins IJ. Autoimmune disease and mitochondrial dysfunction in chronic diseases,Res. Chron. Dis. 1, 1 (2017).
- Turnbull D, Rodricks JV, Mariano GF . Caffeine and cardiovascular health. Regul Toxicol Pharmacol. 89,165-185 (2017).
- Martins IJ. Caffeine consumption with Relevance to Type 3 diabetes and accelerated brain aging. Research and Reveiws Neuroscience. 1, 1-5 (2016).
- Martins IJ. Nutrition Therapy Regulates Caffeine Metabolism with Relevance to NAFLD and Induction of Type 3 Diabetes. J Diabetes Metab Disord. 4, 19 (2017).
- Martins IJ. Caffeine with Links to NAFLD and Accelerated Brain Aging, Chapter Non-Alcoholic Fatty Liver Disease Molecular Bases, Prevention and Treatment. In Tech Open. (2017).
- Martins IJ. Food intake and caffeine determine amyloid beta metabolism with relevance to mitophagy in brain aging and chronic disease. EJFST. 4, 11-17 (2016).
- Martins IJ. Functional Foods and Active molecules with relevance to Health and Chronic disease. Functional Foods in Health and Disease. 7, 833-836 (2017).