Research Article - Diabetes Management (2018) Volume 8, Issue 6
Self management ability mediates the relationship of diabetes mellitus patients activeness in prolanis with their quality of life
- *Corresponding Author:
- Novelasari
- Department Health Promotion
Poltekkes Kemenkes RI Padang, West Sumatera Province, Indonesia
E-mail: rapitossiddiq@gmail.com
Abstract
Objectives: Diabetes mellitus is still a problem in the world today, including Indonesia because of the complications it causes. Various forms of health programs were launched to overcome them, one of which was prolanis with the aim of improving the self-management and quality of life of patients. The purpose of the study is to identify self management effect in mediating the relationship of diabetes mellitus patients’ activeness in prolanis with their quality of life. Methods: This is a analytical study with a cross sectional design. The data was collected on May 20 to June 3, 2018, using the WHOQOL-BREF questionnaire to 52 respondents. The data were analyzed using path analysis based on linear regression. Results: Results showed that 68% of respondents have good quality of life are those who actively participate in prolanis, 91% of respondents who have a good quality of life are those who have good self-management. According to the path value between the respondents activeness with their quality of life directly was 0.364 (P1=0.364), the relationship between the respondents activeness with their self management was 0.438 (P2=0.438), and the path value between respondents self management with their quality of life directly is 0.355 (P3=0.355). The amount of indirect effect is 0.438 x 0.355 = 0.155 (0.155<0.364) thus the indirect relationship coefficient is still smaller than the direct relationship. Conclusions: The study prove that self-management does not have the ability to mediate the relationship of diabetes mellitus patients activeness in prolanis with their quality of life, or self-management is not a mediator factor but a factor that directly contributes to the quality of life of patients.
Keywords
prolanis, patients’ activeness, self-management, diabetes mellitus, quality of life
Introduction
Diabetes mellitus is a non-communicable disease that poses a serious threat to health development. The disease is a public health problem both globally, regionally, nationally and even locally because the complications can result such as blindness, kidney failure, gangrene, heart disease and stroke [1]. Therefore, it needs an effort to overcome it, one of which is a service program for chronic disease (called prolanis). Prolanis is a health service system and a proactive approach that is implemented in an integrated manner. One of the diseases targeted by this program is type 2 diabetes mellitus. The program involves participants, health care facilities and the Health Insurance Service Agency (called BPJS Health). This service is intended to maintain health of participants who suffer from chronic diseases. They are expected to achieve optimal quality with an indicator that 75% of participants visiting first-level health care facilities have “good” results on specific tests for diabetes mellitus effectively and efficiently so as to prevent complications of the disease. Prolanis activities include activities for medical consultations or education and home visits to provide personal and environmental health information for prolanis participans and families. Prolanis also has a reminder program via SMS Gateway to motivate participants in access health service information, status of club and health care [2]. Quality of life is not only related to physical conditions but also psychological / mental health. In general, the quality of life (quality of life, QoL or QOL) is the quality that is felt in the daily lives of individuals, namely an assessment of their welfare or lack thereof. This covers all emotional, social, and physical aspects in the lindividuals lives [3]. Based on the observations of researchers in early July 2017 in the big cities of Banda Aceh and Aceh, there were several health centers and pre-primary health care facilities (called puskesmas) that had implemented prolanis, such as Baiturrahman, Ulee Kareng, Kuta Alam, Ingin Jaya and Lambaro Meurasi Clinic. Of the first level health facilities that researchers observe, Lambaro Meurasi Clinic is one of the first premedical health care facilities that have been actively carrying out prolanis since 2013. Based on secondary data from prolanis managers, the number of registered participants up to January 2018 was more than 60 people. The activities are held every Sunday, precisely in first and third week. The activities forms are health counseling; morning exercise; examination of blood sugar levels (called KGD) and blood pressure; laboratory test (in collaboration with the prodia); and home visits. Since researchers began to be participants in prolanis (early January 2018), researchers found the fact that not all participants actively and they often come in turns. This condition lasted until this research was carried out. From the results of interviews conducted by researchers in early March 2018 with 5 participants revealed that they already knew the condition of the illness. They also knew what actions must be taken to reduce the severity of the disease, especially those related to KGD. They have positive and constructive coping attitudes, are always upbeat and optimistic. Some participants, who actively acknowledge that they can share experiences, gather with friends in pain, empathize and motivate to keep their spirit alive. However, the inactive participants admitted that they were afraid when the KGD examination would be carried out, they were afraid that the results would be bad so they thought it would be better not to be examined at all. Researchers also found that some participants were unable to complete morning exercise due to fatigue, body aches, lackluster and unstable KGD. This shows that they have problems in managing the disease so that it has an impact on quality of life. This condition found in early May 2018. Based on preliminary research, it was found that active prolanis participants had the ability to manage their disease well. They get the ability from their experience in following prolanis. This is supported by several results of studies such as Primahuda and Sujianto, found a relationship between prolanis adherence to the stability of blood sugar among patients at Babat Health Center (Lamogan Regency), so that this program can be used as a reference for people with diabetes to improve compliance so that diabetes patients have sugar stable blood [4]. And Dewi Ratih et al. found an association between blood glucose levels and the quality of life of patients with type 2 diabetes mellitus who were recorded in prolanis as well as health insurance participants in Surakarta [5]. so the researchers question whether the activeness of participants following prolanis directly has an impact on the quality of life, or precisely the activeness of the participants have formed a good self-management so that it has been able to improve the quality of life. Based on these problems the purpose of the study is to identify self-management effect in mediating the relationship of diabetes mellitus patients activeness in prolanis with their quality of life.
Methods
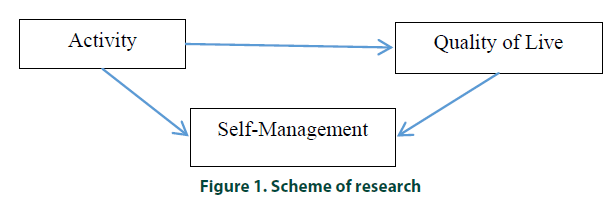
This study used cross sectional method in analytical descriptive type of research. This research was carried out at the General Meurasi Lambaro Clinic in Aceh Besar District, Aceh Province. The samples were patients with diabetes who follow prolanis actively. A sample of 52 respondents was calculated using the total sampling. To assess the activity of patients using secondary data from attendance of prolanis participants, while to assess self-management was measured by using a questionnaire and measuring the quality of life using the WHOQOL-BREF questionnaire. Data is collected on May 20 to June 3, 2018. Data processing stages are; editing, coding, transfering and tabulating. Data analysis uses linear regression path analysis. In summary, the research scheme can be described as follows in Figure 1.
Results
Characteristics of respondents in terms of age, sex, level of education, length of illness, and length of following prolanis based on respondents activeness, self-management and quality of life. In detail it is illustrated in the Tables 1-3 below:
▪ Characteristics of respondents and activeness in prolanis
Characteristics of respondents were reviewed in terms of age, sex, level of education, length of illness, and length of following prolanis based on respondents activeness (Table 1). Based on the table above it is known that of 52 respondents, activeness were dominated by the age group of 45-60 years as many as 14 people (48.3%), female as many as 14 people (53.8%), high education as many as 15 people (53.6%), length of illness 1 -5 years as many as 14 person (56.0%). Whereas those who were less active in following prolanis activities were dominated for a period of 1 to 2 years in prolanis as many as 20 people (55.6%).
| Characteristics | n | % | Self-management | ||||
|---|---|---|---|---|---|---|---|
| Good | % | Poor | % | ||||
| <45 years | 5 | 9.6 | 4 | 80 | 1 | 20 | |
| Age | 45-60 years | 29 | 55.8 | 12 | 41.4 | 17 | 58.6 |
| >60 years | 18 | 34.6 | 7 | 38.9 | 11 | 61.1 | |
| Male | 26 | 50 | 12 | 46.2 | 14 | 53.8 | |
| Sex | Female | 26 | 50 | 11 | 42.3 | 15 | 57.7 |
| Level of education | Basic | 2 | 3.8 | 1 | 50 | 1 | 50 |
| Middle | 22 | 42.3 | 11 | 50 | 11 | 50 | |
| High | 28 | 53.8 | 11 | 39.3 | 17 | 60.7 | |
| <1 years | 2 | 3.8 | 0 | 0 | 2 | 100 | |
| Length of | 1-5 years | 25 | 48.1 | 11 | 44 | 14 | 56 |
| Illness | >5 years | 25 | 52.1 | 13 | 48 | 12 | 48.1 |
| Length of following prolanis | <1 years | 3 | 5.8 | 2 | 66.7 | 1 | 33.3 |
| 1-2 years | 36 | 69.2 | 14 | 38.9 | 22 | 61.1 | |
| >2 years | 13 | 25 | 7 | 53.8 | 6 | 46.2 | |
Table 1. Characteristics of respondents and activeness in prolanis
▪ Characteristics of respondents and conditions of self-management
Characteristics of respondents were reviewed in terms of age, sex, level of education, length of illness, and length of following prolanis based on self-management conditions in Table 2. Based on the table above it can be seen that from 52 respondents, poor self-management conditions were found in the age group 45-60 as many as 17 people (58,6%), female as many as 15 people (57,7%); high education as many as 17 people (60.7%), and found in the group following prolanis 1-2 years as many as 22 people (61.1%). On the other hand, is found to be almost balance frequency between good and poor selfmanagement for 1-5 years of illness with more than 5 years.
| Characteristics | n | % | respondents activeness | ||||
|---|---|---|---|---|---|---|---|
| Active | % | Less active | % | ||||
| <45 years | 5 | 9.6 | 4 | 80 | 1 | 20 | |
| Age | 45-60 years | 29 | 55.8 | 14 | 48.3 | 15 | 51.7 |
| >60 years | 18 | 34.6 | 7 | 38.9 | 11 | 61.1 | |
| Male | 26 | 50 | 11 | 42.3 | 15 | 57.7 | |
| Sex | Female | 26 | 50 | 14 | 53.8 | 12 | 46.2 |
| Level of education | Basic | 2 | 3.8 | 0 | 0 | 2 | 100 |
| Middle | 22 | 42.3 | 10 | 45.5 | 12 | 54.5 | |
| High | 28 | 53.8 | 15 | 53.6 | 13 | 46.4 | |
| <1 years | 2 | 3.8 | 0 | 0 | 2 | 100 | |
| Length of | 1-5 years | 25 | 48.1 | 14 | 56 | 11 | 44 |
| Illness | >5 years | 25 | 48.1 | 11 | 44 | 14 | 56 |
| Length of following prolanis | <1 years | 3 | 5.8 | 2 | 66.7 | 1 | 33.3 |
Table 2. Characteristics of respondents and self-management conditions
▪ Characteristics of respondents and quality of life
Characteristics of respondents were reviewed in terms of age, sex, level of education, length of illness, and length of following prolanis based on quality of life in Table 3. Based on the table above it is known that the majority of respondents who have good quality of life aged 45-60 years as many as 17 people (58.6%), male as many as 16 people (61.5%), high education as many as 17 people (60.7%), length of illness of more than 5 years as many as 12 people (54.5%). Whereas those who were poor quality of live in following prolanis activities were dominated for a period of 1 to 2 years in prolanis as many as 22 people (61.1%).
| Characteristics | n | % | Quality of life | ||||
|---|---|---|---|---|---|---|---|
| Good | % | Poor | % | ||||
| <45 years | 5 | 9.6 | 4 | 80 | 1 | 20 | |
| Age | 45-60 years | 29 | 55.8 | 17 | 58.6 | 12 | 41.4 |
| >60 years | 18 | 34.6 | 9 | 50 | 9 | 50 | |
| Sex | Male | 26 | 50 | 16 | 61.5 | 10 | 38.5 |
| Female | 26 | 50 | 14 | 53.8 | 12 | 46.2 | |
| Level of education | Basic | 2 | 3.8 | 1 | 50 | 1 | 50 |
| Middle | 22 | 42.3 | 12 | 54.5 | 10 | 45.5 | |
| High | 28 | 53.8 | 17 | 60.7 | 11 | 39.3 | |
| Length of | <1 years | 2 | 3.8 | 1 | 50 | 1 | 50 |
| 1-5 years | 25 | 48.1 | 13 | 52 | 12 | 48 | |
| >5 years | 25 | 48.1 | 16 | 64 | 9 | 36 | |
| Length of following prolanis | <1 years | 3 | 5.8 | 2 | 66.7 | 1 | 33.3 |
| 1-2 years | 36 | 69.2 | 14 | 38.9 | 22 | 61.1 | |
| >2 years | 13 | 25 | 7 | 53.8 | 6 | 46.2 | |
Table 3. Respondent characteristics and quality of life
▪ Comparison of the activeness and selfmanagement to quality of life
The Table 4 shows that the majority of respondents who have a good quality of life (68.0%) are active in prolanis and have good self-management (91.3%).
| Quality of life | Total | |||||
|---|---|---|---|---|---|---|
| Good | % | Poor | % | |||
| Activeness | Active | 17 | 68 | 8 | 32 | 25 |
| Less active | 13 | 48.15 | 14 | 51.85 | 27 | |
| Self Management | Good | 21 | 91.3 | 2 | 8.7 | 23 |
| Bad | 9 | 31.03 | 20 | 68.97 | 29 | |
Table 4. Comparison of the activeness and self-management of quality of life
▪ Path analysis
Path analysis based on linear regression is used to identify the relationship between the two independent variables (activeness and selfmanagement) with the dependent variable (quality of life). The analysis produces the following data in (Table 5). Path analysis results in the table above show that the standarized coefficient of respondent activeness is 0.364 which means that the path value between the respondent’s activeness to the quality of life directly is 0.364 (P1=0.364), and the path value (path) between self-management to the quality of life directly is 0.355 (P3=0.355, so the regression model that is formed is:
Y = 23.958 +0.108 activeness + 0.355 self- management + e
| Coefficientsa | ||||||
|---|---|---|---|---|---|---|
| Model | Unstandardized Coefficients | Standardized Coefficients | T | Sig. | ||
| B | Std. Error | Beta | ||||
| 1 | (Constant) | 23.958 | 2.441 | 9.813 | 0 | |
| activeness | 0.108 | 0.037 | 0.364 | 2.887 | 0.006 | |
| self management | 0.159 | 0.056 | 0.355 | 2.815 | 0.007 | |
a. Dependent Variable: Quality of life
Table 5. Pathway relationship analysis between variables
The magnitude of the relationship between the variables of activeness to self-management as an intervening variable with path analysis based on linear regression, the following results are obtained in (Table 6). From the table it can be seen that the standarized coefficients activeness variable is 0.438, meaning that the relationship between activeness to self-management is 0.438 (P2=0.438), so the regression model that is formed is:
Y = 39.190 + 0.289 activeness + e
| Coefficientsa | ||||||
|---|---|---|---|---|---|---|
| Unstandardized Coefficients | Standardized Coefficients | T | Sig. | |||
| Model | B | Std. Error | Beta | |||
| 1 | (Constant) | 39.19 | 2.589 | 15.135 | 0 | |
| Keaktifan Responden | 0.289 | 0.084 | 0.438 | 3.449 | 0.001 | |
Table 6. Pathway analysis of intervening variable relations
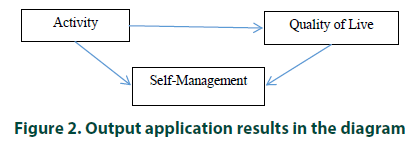
Based on two path analysis results in the tables above, it can be illustrated the relationship diagram between complete variables with path values as follows in Figure 2. Based on the results of processing the data above, it can be seen that the activeness directly affects the quality of life of respondents. However, these variables can also affect the quality of life of respondents indirectly by means of self-management variables as intervening variables. The amount of indirect effect can be calculated as follows:
0.438 x 0.355 = 0.155 (0.155 <0.364)
Thus the indirect relationship coefficient is still smaller than the direct relationship. So it can be concluded that the relationship between variables in this case is a direct relationship, meaning that although there is no self-management variable, the activeness variable still influences the quality of life of the respondents, so the ability of self-management mediates the relationship of respondents in the prolanis with the quality of life of the Diabetes mellitus respondents cannot be proven.
Discussion
The quality of life of the patient or community is a very important indicator in assessing health care programs [6]. Moreover, the activeness of patients or community is a strategic factor in supporting a successful health program. The results of this study found that the majority (68%) of respondents who had a good quality of life were those actively following prolanis (Table 4). In other words, the activeness of participants following prolanis can affect the quality of life. This is because participants follow many activities in prolanis, such as health education, medical consultations, KGD examination, healthy exercise and home visits. Through this activity, participants can also socialize with each other to share experiences in handling their illness. These things certainly at least have provided moral support among participants in improving physical and mental health conditions. Furthermore, their quality of life has improved, despite many other factors that can be used to assess quality of life, such as meeting physical needs and socioeconomic conditions[7], but health is a very important factor. A study shows that the socialization or meeting of diabetics patiens is very important in improving the mental health of participants [8]. Quality of life is an individual’s view of the comparison of the quality of life with his desires, measured in terms of physical health, psychological conditions, social relations, and the environment [3]. Quality of life is also influenced by demographic and medical factors. Socio demographic factors as gender, age, ethnicity or ethnicity, education, occupation and marital status. Medical factors are length of therapy, stage of illness, and medical management. The comparison with the results of this study clearly illustrates that in terms of age more than 90% of respondents aged 45 years and over and 53% were highly educated. Age factors greatly affect once the quality of life of participants, which age 45 years and over is the age of having emotional maturity which will greatly affect perceptions and attitudes, especially in adjusting themselves to the condition of the disease. Likewise with the education factor, higher education is certainly a big asset for participants to obtain information in recognizing their illness and knowledge in the effort to handle the disease. These two demographic factors strongly support participants to achieve a good quality of life. In the medical aspect, this study found two factors that were very supportive i.e length of illness and length of following prolanis. In this study, most of the respondents had participated in prolanis for more than 2 years, which was dominated by people with diabetes mellitus for more than 1 year (96.2%). This also greatly influenced the creation of a good quality of life. Participants’ activeness in prolanis indirectly has actually formed good self-management. The activeness and selfmanagement are two interrelated factors. This study found a significant relationship between the respondents activeness with self-management with a value of sig. 0.001 (<0.05) (Table 6). The relationship between the respondent’s activeness in prolanis and self-management has formed an ability to organize themselves, manage a lifestyle that is in accordance with the demands of the management of the disease. Health education or counseling activities contained in prolanis, is an ongoing process of facilitating the knowledge, skills and abilities needed for self-care of diabetic patients. This process combines needs, goals and life experiences. The education forms selfmanagement so as to support decision making, self-care behavior, problem solving, working with health care teams and to improve the quality of clinical outcomes of KGD, health status, and quality of life [9]. Self-management for diabetes mellitus patients is referring to several activities i.e monitoring signs and symptoms, maintaining and improving health behavior, and overcoming the negative effects of the disease on the patient’s physical function, emotional feelings, and interpersonal relationships [10]. The results of study confirm that the key to preventing diabetes is to change the lifestyle of patients [11]. The importance of this self-management for diabetes mellitus patients has an impact on the control of KGD [12-15] There have been many studies that prove that self-management education has an impact on increasing respondents’ knowledge, KGD monitoring frequency and accuracy, and dietary settings [15,16]. Apart from the existence of a significant relationship between the diabetes mellitus patients activeness with their quality of life and a significant relationship between their activeness and self-management. This study did not find a significant influence on self-management factors in supporting the relationship between respondents activeness in prolanis with their quality of life. Even though the better self-management of respondents increased the quality of life as well, as shown in Table 4, it was illustrated that 91.30% of respondents who had good self-management and had a good quality of life as well, whereas 68.97% of respondents who had self-management and were not good have a bad quality of life too. In this case, the activeness in following prolanis activities more significantly improves the quality of life of diabetes mellitus patients. Research shows that health education programs followed by diabetic patients are very important to diabetes control. Health education able to increase the knowledge of diabetic patients and increase their awareness. Health education is suitable for various ages, by participants to shape good self-management and have an impact on the quality of life of patients. This program is recognized as effective in promoting better diabetes care and positively influencing self-care behaviors associated with glycemia and diabetes. However it requires time, commitment and careful coordination with many professional nurses [18]. Otherwise prolanis has been able to manage the potential possessed by participants to form good selfmanagement and have an impact on the quality of life of patients. Based on the facts found in this study, self-management can be viewed from two sides. On the one hand, self-management is the dependent variable when faced with patient activeness variables as independent variables. Self-management can act as an independent variable that affects the quality of life of patients. Emphasis in this study is that self-management cannot be used as a mediating or intervening factor in looking at the relationship between diabetes mellitus patiens activeness and their quality of life, but self-management is actually a factor that directly affects the quality of life of diabetes mellitus patients.
Study Limitations
This study was conducted with a small sample size, without observing differences in selfmanagement and quality of life among groups of patients with diabetes mellitus who followed prolanis with those who did not. Therefore, more advanced research is recommended.
Conclusion
The study prove that self management does not have the ability to mediate the relationship of diabetes mellitus patients activeness in prolanis with their quality of life, or self-management is not a mediator factor but a factor that directly contributes to the quality of life of patients.
References
- Center for Public Communication Secretariat General of the Ministry of Health of the Republic of Indonesia, "Diabetes mellitus is the number six cause of death in the world; The Ministry of Health offers smart solutions through guidance posts" Ministry of Health of the Republic of Indonesia, 2013. www.depkes.go.id.
- BPJS, Prolanis practical guide (Chronic disease management program). Jakarta: BPJS Health, 2014.
- WHO, “WHOQOL measuring Quality of life,” in Programme On Mental Health, Switzerland: Division of mental health and Prevention of substance abuse. 1–13 (1997).
- Primahuda A, Sujianto U. The relationship between adherence to follow Prolanis with stability of blood sugar in people with diabetes. Jurnal-Keperawatan Fak. Kedokteran, Univ. Diponegoro Semarang, 13, 2016.
- Dewi R, Romadhon Y, Candrasari A. Relationship between blood glucose patients with Diabetes mellitus type 2 and quality of life among Prolanis Askes participants at Surakarta. Universitas Muhammadiyah Surakarta, (2014).
- Pakpour A, Saffari M, Yekaninejad M et al. Health-related quality of life in a sample of ıranian patients on hemodialysis. Iran. J. Kidney. Dis. 4 (1), 50–59 (2010).
- Robert C, Brendan F, Saleem A et al. Quality of life: An approach integrating opportunities, human needs, and subjective well-being. Ecol. Econ. 61 (2–3), 267–276 (2007).
- Ventegodt S, Merrick J, Andersen N. Quality of life theory I. The IQOL theory: An ıntegrative theory of the global quality of life concept. Sci. World J. 13(3), 1030–1040, 2003.
- Linda H, Melinda M, Joni B et al. National standards for diabetes self-management education. Diabetes Care. 35 (11), 2393–2401 (2012).
- Huang M, Zhao R, Li S et al. Self-management behavior in patients with type 2 diabetes: A cross-sectional survey in western urban China. PLoS One 9(4), e95138 (2014).
- J. Tuomilehto. Type 2 diabetes ıs a preventable disease - lifestyle ıs the key. J. Med. Sci. 3(2), 82–86 (2010).
- Iunes D, Rocha C, Borges N et al. Self-care associated with home exercises in patients with type 2 diabetes mellitus. PloS. One. 9(12), e114151 (2014).
- H. Holman, K. Lorig. Patient self-management : A key to effectiveness and efficiency in care of chronic disease. Public. Health. Rep. 119(3), 239–243 (2004).
- Yu C, Parsons J, Mamdani M et al. A web-based intervention to support self-management of patients with type 2 diabetes mellitus: Effect on self-efficacy, self-care and diabetes distress. BMC Med. Inform. Decis. Mak. 14(1), 117 (2014).
- Norris S, Engelgau M, Narayan M. Effectiveness of self-management training in type 2 diabetes-a systematic review of randomized controlled trials. Diabetes. Care. 24 (3), 561–587 (2001).
- Ferguson S, Swan M, Smaldone A. Does diabetes self-management education in conjunction with primary care ımprove glycemic control in hispanic patients?: A systematic review and meta-analysis, Diabetes. Educ. 41(4), 472–484 (2015).
- Osman M, Ahmed E, Ahmed H. Effects of health education of diabetic patient’s knowledge at diabetic health centers, Khartoum State, Sudan: 2007-2010. Glob. J. Health Sci. 6(2), 221–226 (2014).
- Polonsky W, Earles J, Smith S et al. Integrating medical management with diabetes self-management training. Diabetes. Care. 26(11), 3048–3053