Case Report - Diabetes Management (2017) Volume 7, Issue 5
Coexistence of insulin induced acanthosis and lipoatrophy in a patient with type 1 DM
- *Corresponding Author:
- Bengur Taskiran
Department of Endocrinology
Yunus Emre State Hospital
Eskisehir, Turkey
E-mail: bengurtaskiran@yahoo.com.tr
Abstract
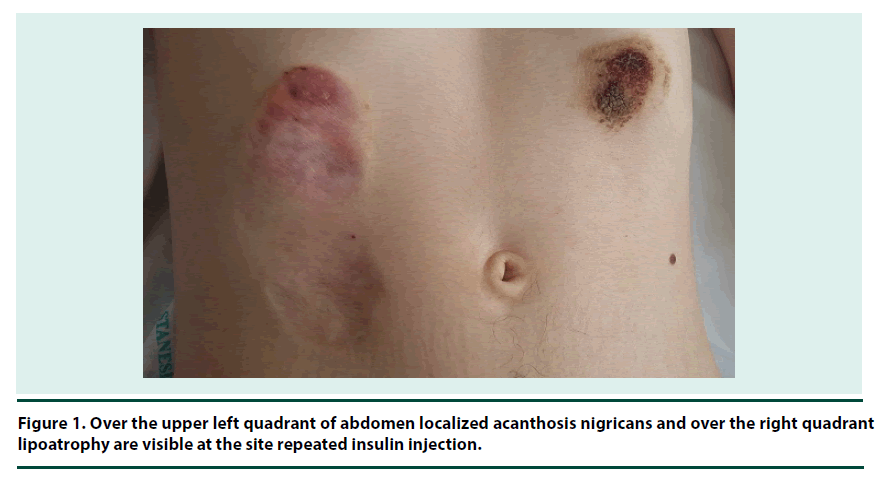
Localized acanthosis nigricans at the insulin injection site is a rare skin disorder in patients with diabetes mellitus. We report co-existence of acanthosis nigricans and lipoatrophy at injection sites in the same patient with type 1 DM. A 23 year old male patient with a history type 1 DM for 11 years was admitted to hospital due to recurrent diabetic ketoacidosis attacks. There were two lesions over the abdominal skin which occurred due to repeated insulin injection at the same sites. Despite structured and continuous education even in developed countries, poor injection technique still remains a challenging factor in uncontrolled diabetes mellitus. Injection sites should be checked for localized acanthosis nigricans in addition to lipodystrophy. There is no other report in the literature regarding coexistence of both lipoatrophy and localized acanthosis nigricans in the same patient with type 1 diabetes mellitus.
Keywords
acanthosis nigricans, lipoatrophyprimary care, insulin, type 1 diabetes mellitus
Introduction
There is a variety of cutaneous reactions induced by insulin administration at the injection site including hyperemia, pruritus, lipoatrophy, lipohypertrophy, infection, folliculitis, cheloid, and acanthosis nigricans (AN) [1]. Lipoatrophy and lipohypertrophy are collected under the name of local lipodystrophy. Lipodystrophy is thickening of subcutaneous tissue giving a feeling for rubbery mass. Lipoatrophy is characterized with depressed paper like skin due to loss of subcutaneous tissue. Lipodystrophy is a common manifestation (up to 50% in different series) even in developed countries despite purity of insulin preparations and burden of knowledge regarding good injection technique [2,3]. Lipoatrophy is more common in type 1 DM and lipohypertrophy in type 2 [2]. Lipodystrophy may occur with both human and analogue insulins. Number of daily injection, duration of diabetes, duration of insulin therapy, reuse of needles, and needle size are contributors of lipodystrophy probably due to intensity of trauma to subcutaneous tissue [2].
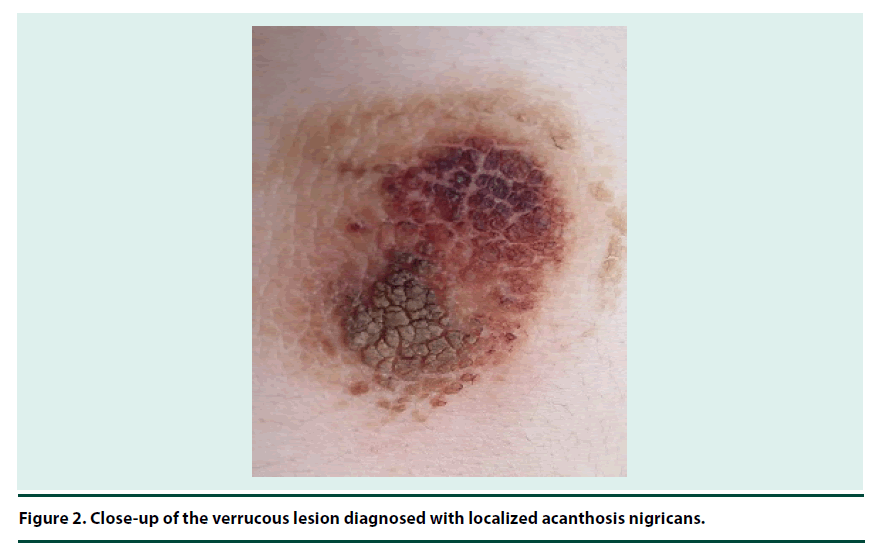
AN is rarely encountered at the site of injection. AN is a dermatosis commonly observed in diseases associated with insulin resistance including type 2 DM, obesity, and polycystic ovary syndrome and rarely accompany malignancies [4,5]. AN is characterized by velvety texture, commonly hyperpigmented and brownish in colour, and verrucous structure which gave an impression of dirty appearance [4]. It may involve skin of intertriginous areas (armpits, antecubital fossae, folds of the neck, between digits, beneath the breasts, and groin) and less commonly mucosa, palms and soles [4].
A few cases of localized AN associated with insulin usage have been reported in the literature [6]. There is no report in English written language regarding coexistence of lipodystrophy and AN in a patient with type 1 DM.
Case Report
A 23 year old male patient, who had type 1 DM for 11 years, was admitted to the endocrinology ward because of nausea and vomiting. He was diagnosed with diabetic ketoacidosis (DKA). He denied any other chronic illness. He was suffering from frequent hospitalizations due to ketoacidosis. He was on 14 U glargine once a day and 10 U aspart insulin thrice a day before meals therapy and not using other medications or herbal products. He was a current smoker. He was using prefilled pens and 32 G needles. On physical examination a brown-coloured verrucous lesion measuring approximately 4 cm in diameter over the upper left quadrant of abdomen (Figure 1) and a 10 x 3 cm area of thinned paper-like skin over the right quadrant of upper abdomen were noted (Figure 2). He weighed 44.7 kg and was 170 cm tall. Neither lipoatrophy nor AN were present elsewhere in the body except the aforementioned site. The site of AN was atypical for that observed in insulin resistance disorders including malignancy. He used to rotate only upper quadrants of abdomen interchangeably for insulin injection. Therefore localized AN and lipoatrophy due to incorrect insulin injection pattern were diagnosed.
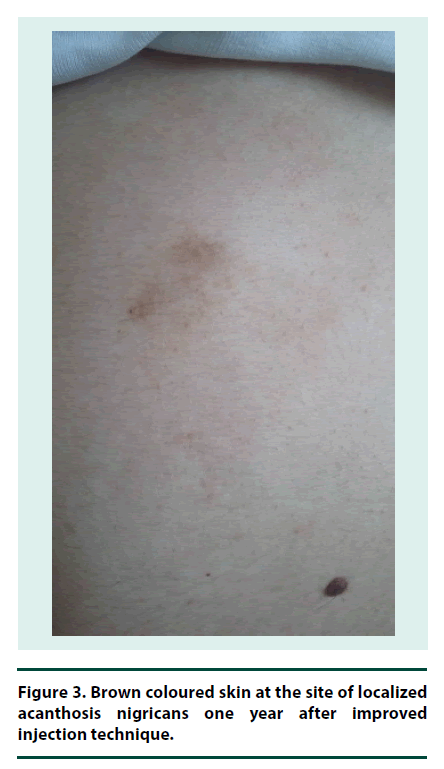
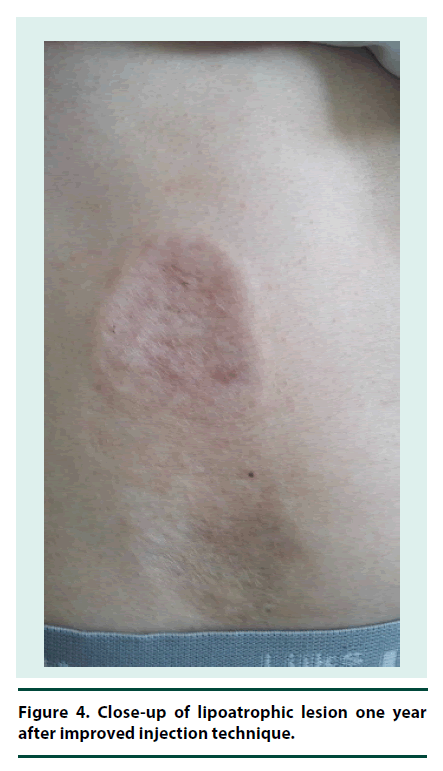
He refused excisional biopsy of the lesion. Renal and liver function tests were normal; hemoglobin A1C was 57 mmol/mol (7.4%); antibodies against TPO, endomysium, and gliadin were negative, microalbuminuria was absent, TSH and vitamin B12 levels were normal. Fundus examination was normal. He suffered from frequent DKA attacks probably due to poor absorption of insulin. Therefore to decrease the number of injections, avoid metal needle trauma, and fine tune insulin dosage, we switched multiple day injection therapy to continuous subcutaneous aspart insulin infusion using soft silicone infusion set. The lesions were persisting at the 5th month of follow-up. One year after follow-up by two medical centers (Yunus Emre State hospital and Osmangazi University), he was doing well and had hemoglobin A1C level of 43 mmol/mol (6.1%). Localized acanthosis nigricans disappeared with slight brownish colour at the site of the lesion (Figure 3). However right-sided lipoatrophy persisted despite improvement (Figure 4). He has still avoids abdomen as injection site for CSII.
Discussion
We present the first case of co-existence of two dermatoses (AN and lipodystrophy) due to repeated injection of insulin to the same sites in a patient with type 1 DM.
Local lipodystrophy (lipoatrophy and lipohypertrophy) at the sites of insulin injection mostly occurs with porcine or bovine derived insulin, but it may also be due to human or analogue insulins administered by needle or subcutaneous infusion systems [7]. It takes 4 weeks to 2 years for lipodystrophy to develop. Neglecting rotation of sites for insulin injection is a frequent cause. Degenerative changes in adipose tissue and IgM, complement, and fibrin-fibrinogen deposition in dermal vessels of neighbouring tissue suggest an immune mediated inflammatory reaction [7]. Injected insulin and antibody developed against exogenous insulin forms a complex which in turn activates complement formation and resultant infiltration with inflammatory cells [7]. Cytokines secreted from mastocytes may inhibit adipocyte differentiation [7]. Lipoatrophy has immunulogic basis and impurity of insulins may contribute lipolytic reaction [2]. On the other hand lipohypertrophy is due to lipogenic activity of insulin and hypertrophy of subcutaneous adipocytes replace mid derm collagen leading to thickened skin [2]. Poor injection technique due to avoiding rotation and injecting repeatedly at the same site is the most common cause [2]. Both atrophy and hypertrophy may cause erratic glucose levels due to impaired insulin reabsorption [2].
The diagnosis of AN can be made easily on clinical grounds and histopathological examination confirms the diagnosis. Our patient refused the biopsy of lesions. Therefore we are unable to show structural changes in dermis and subcutaneous tissue. However the microscopic features of localized AN have already been defined in the literature. The diagnosis of AN can be made easily on clinical grounds and histopathological examination confirms the diagnosis. Our patient refused the biopsy of lesions. Therefore we are unable to show structural changes in dermis and subcutaneous tissue. However the microscopic features of localized AN have already been defined in the literature. Pathophysiologic data regarding AN are derived from studies executed in genetically determined insulin resistance syndromes and fibroblast growth factor (FGF) defects [4]. Normal epidermal cells especially the actively proliferating cells of the basal layer present epidermal growth factor receptor (EGFR) [8]. Basal layer is involved in growth and differentiation of normal keratinocytes [8]. Keratinocytes comprise 95% of epidermal cells and arise from the basal layer of epidermis. Keratinocytes migrate into the upper epidermal layers. Aside from their structural role, keratinocytes also exert immunological activity via release of cytokines. There is marked hyperkeratosis and papillary hypertrophy of the basal layer of epidermis in haematoxylin eosin stained skin tissue.8 Antibodies directed against IGF receptor and EGFR expressed by fibroblasts and keratinocytes might play a role in the pathogenesis of AN [4]. Amyloid deposits may accompany other characteristic histological findings of AN [9]. Transforming growth factor (TGF)-α acting via (epidermal growth factor receptor (EGFR)), insulin-like growth factor (IGF)-1, fibroblast growth factor (FGF), and melanocyte stimulating hormone-α (MSH-α) play a role in melanocyte pigmentation and growth of keratinocytes, which in turn may lead to AN [8,10].
A large survey done in 500 patients with type 1 DM revealed exogenous insulin related localized AN only in 2 patients [1]. In the literature all reported cases are male patients with either type 1 or type 2 DM, aged between 14-73 years [6,9- 12]. Duration of insulin administration varies between 4 to 10 years. Malrotation is the major cause in all. The first case in the literature was due to beef pork insulin usage. Other cases are due to human recombinant regular and NPH insulin, except one with glargine and aspart insulin.
In many health facilities diabetes nurses and doctors provide structured education about insulin therapy. Despite all efforts, the patients may not adhere to the instructions. This case represents a good example of different skin reactions occurring in the same patient due to exogenous insulin.
Conclusion
The patients with poor glycaemic control, erratic course, and frequent hospitalizations should be sought for proper injection and related cutaneous pathologies including localized AN and lipodystrophy.
References
- Sawatkar GU, Kanwar AJ, Dogra S et al. Spectrum of cutaneous manifestations of type 1 diabetes mellitus in 500 South Asian patients. Br. J. Dermatol. 171(6), 1402–1406 (2014).
- Hajheydari Z, Kashi Z, Akha O et al. Frequency of lipodystrophy induced by recombinant human insulin. Eur. Rev. Med. Pharmacol. Sci. 15(10), 1196–1201 (2011).
- Gentile S, Guarino G, Giancaterini A, et al. AMD-OSDI Italian Injection Technique Study Group A suitable palpation technique allows to identify skin lipohypertrophic lesions in insulin-treated people with diabetes. Springerplus. 5(1), 563 (2016).
- Torley D, Bellus GA, Munro CS. Genes, growth factors and acanthosis nigricans. Br. J. Dermatol. 147(1), 1096–1101 (2002).
- Stulberg DL, Clark N, Tovey D. Common hyperpigmentation disorders in adults: Part II. Melanoma, seborrheic keratoses, acanthosis nigricans, melasma, diabetic dermopathy, tinea versicolor, and postinflammatory hyperpigmentation. Am. Fam. Physician. 68(10), 1963–1968 (2003).
- Yahagi E, Mabuchi T, Nuruki H et al. Case of exogenous insulin-derived acanthosis nigricans caused by insulin injections. Tokai. J. Exp. Clin. Med. 39(1), 5–9 (2014).
- Kadiyala P, Walton S, Sathyapalan T. Insulin induced lipodystrophy. Br. J. Diabetes Vasc. Dis. 14(1), 131–133 (2014).
- Phiske MM. An approach to acanthosis nigricans. Indian Dermatol Online J. 5(3), 239-249 (2014). doi: 10.4103/2229-5178.137765.
- Kudo-Watanuki S, Kurihara E, Yamamoto K et al. Coexistence of insulin-derived amyloidosis and an overlying acanthosis nigricans-like lesion at the site of insulin injection. Clin. Exp. Dermatol. 38(1), 25–29 (2013).
- Buzási K, Sápi Z, Jermendy G. Acanthosis nigricans as a local cutaneous side effect of repeated human insulin injections. Diabetes Res. Clin. Pract. 94(2), e34–e36 (2011).
- Sawatkar GU, Dogra S, Bhadada SK et al. Insulin injection: cutaneous adverse effects. Indian J. Endocrinol. Metab.19(4), 533–534 (2015).
- Mailler-Savage EA, Adams BB. Exogenous insulin-derived acanthosis nigricans. Arch. Dermatol. 144(1), 126–127 (2008).