Case Report - Interventional Cardiology (2018) Volume 10, Issue 5
Silent coronary rupture treated with coronary emboliza-tion two years after total arch replacement
- Corresponding Author:
- Kazunori Takemura
Department of Cardiology, Ayase Heart, Hospital, Tokyo, Japan
Tel: +81-(0)3-3605-2811
E-mail:kazu880119@gmail.com
Received date: July 07, 2018; Accepted date: June 31, 2018; Published date: August 07, 2018
Abstract
We experienced a case of asymptomatic coronary artery rupture two years after type A acute aortic dissection which was successfully treated with coronary embolization. A 51-year-old man underwent total arch replacement for type A acute aortic dissection two years ago. Although he had been followed uneventfully, follow-up computed tomography scan two years after the operation incidentally identified the hemopericardium compressing the posterolateral wall of the left ventricle. Echocardiography showed significant compression of the left ventricle due to the hemopericardium, but did not show any deterioration of cardiac function. ECG-gated 320-sliced multi-detector computed tomography (MDCT) revealed extravasation from the left circumflex artery. He was hemodynamically stable and asymptomatic despite this potentially life threating condition. After the admission, coronary angiography was performed which revealed coronary artery rupture from the distal part of the second obtuse marginal artery (OM2). The artery was successfully treated with coil embolization. However, four-dimensional computed tomography (4D-CT) three days after the embolization still showed persistent extravasation from the first obtuse marginal artery (OM1). As the artery dominated large areas, OM1 was treated with absorbable gelatin sponge particles. 6 months after the procedures, additional coil embolization was performed for recurrence bleeding from these arteries. After these coil embolization, cardiac enzymes were slightly elevated, but no deterioration of cardiac function was noted and successful hemostasis were achieved. Although considerably rare, asymptomatic coronary artery rupture could happen after the thoracic surgery. 4D-CT is efficient for identifying ruptured sites and coronary embolization is reasonable treatment to achieve hemostasis.
Keywords
Coronary artery perforation, Coronary artery disesase, Coronary embolization, Inteventional cardiology and Four-dimensional computed tomography (4D-CT)
Introduction
.Spontaneous coronary artery rupture (SCAR) is a rare condition and there have been only a few reported cases in the literature [1-3]. Various causes of SCAR have been reported, but all of them have sudden onsets and are critical.
We here report a case of asymptomatic coronary artery rupture which was incidentally diagnosed by follow-up on computed tomography (CT) two years after the surgery for Stanford type A acute aortic dissection. Four-dimensional computed tomography (4D-CT) was efficient for identifying ruptured sites and coronary embolization was proved to be useful for the hemostasis.
Case Report
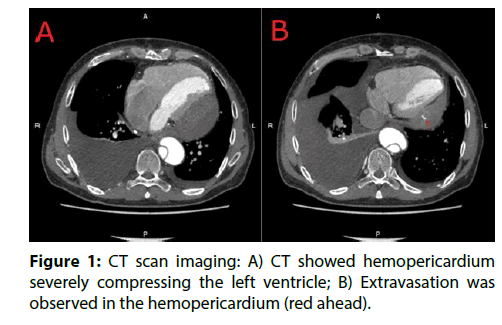
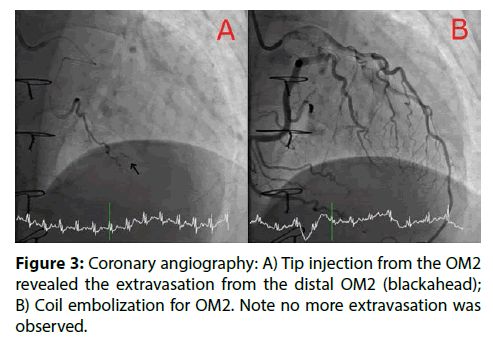
A 51-year-old man had undergone total arch replacement for Stanford type A acute aortic dissection two years ago. Although he had been followed uneventfully at outpatient clinic, the routine follow-up CT scan performed two years after the surgery incidentally identified a hemopericardium (42.2 mm×82.4 mm, CT value 20HU~97.5HU) compressing posterolateral wall of the left ventricle. ECGgated 320-sliced multi-detector computed tomography revealed extravasation into pericardium space (Figure 1). ECG showed a normal sinus rhythm with low voltage of limb leads. Chest X-ray showed cardiomegaly (CTR 55.9%) with left pleural effusion. On echocardiographic assessment, the hemopericardium was severely compressing posterolateral wall of the left ventricle (Figure 2). However, echocardiography showed normal left ventricle function (LVEDV 94.9ml, LVESV 38.2ml, LVEF 59.7%, E/A 1.9 E/med e’ 14.8) and moderate pulmonary hypertension (RVSP 38mmHg, IVC 18mm). With regard to laboratory findings, hypoalbuminemia (Alb 2.4 g/dl), elevated alkaline phosphatase, γ-glutamyl transpeptidase and creatinine kinase (ALP 452 U/L, γ-GTP 219 U/L, Cre 1.23 mg/ dl) were observed. He had no history of traumatic injury, autoimmune diseases such as Kawasaki disease, connective tissue diseases, or infection [4]. Although he had been complaining about bilateral pitting leg edema, he was hemodynamically stable and asymptomatic. After the admission, coronary angiography (CAG) was performed. CAG showed no coronary artery stenosis but extravasation from the distal area of the obtuse marginal arteries. These arteries were tortuous and flow of contrast was observed as to-and-fro pattern which were probably due to the hemopericardium. For hemostasis, coronary embolization was performed. A 6Fr JL4.0 (JL4.0, Launcher, Medtronic Japan, Tokyo, Japan) from right radial artery was positioned in the left main trunk. Using a FINECROSS micro-catheter (Terumo Corp., Tokyo, Japan), a 0.014” SION guide wire (Asahi Intecc Co., LTD., Aichi, Japan) was crossed to the mid part of the first obtuse marginal artery (OM1) after a failed attempt with a Runthrough Extrafloppy (Terumo Corp, Tokyo, Japan). Because of the severe tortuosity, the wire did not pass to the distal site of the branch. Tip injection from the microcatheter on the mid part of the OM1 did not show any extravasation. With similar uses as the OM1, second obtuse marginal artery (OM2) was crossed with SION. Tip injection showed extravasation from the distal part of the OM2. Coil embolization (Hilal Embolization Microcoil 2.0×20 mm×2; Cook Japan, Tokyo, Japan) was successfully performed and no more extravasations were observed from the OM2 (Figure 3). 4D-CT three days after the operation revealed no extravasation from the OM2, but persistent extravasation from the OM1 was observed (Figure 4). We used a 6Fr EBU 4.0 (Launcher, Medtronic Japan, Tokyo, Japan) to improve back up force. At this time, SUOH 03 (Asahi Intecc Co.) with FINECROSS micro-catheter was used to obtain smooth trackability and crossability for this severely tortuous vessel. Tip injection revealed extravasation from the OM1. As the artery dominated a large part of the posterolateral wall of the ventricle, absorbable gelatin sponge particles (Spongel; Astellas Pharma Inc., Tokyo, Japan) were used for hemostasis.
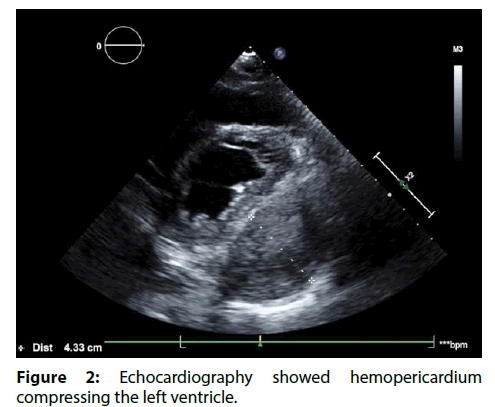
Figure 2: Echocardiography showed hemopericardium compressing the left ventricle.
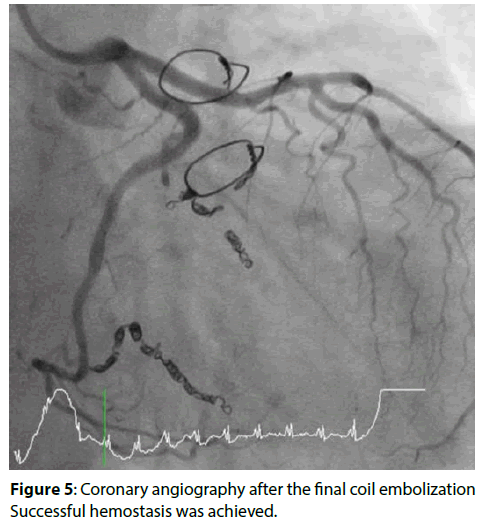
Unfortunately, coronary angiography after 6 months of the operation showed recurrence of bleeding from both of the obtuse marginal. Additional coil embolization (Target XL 2.0×20 mm×3,2.0×30 mm×3; Stryker, Tokyo, Japan) was performed and no more extravasation was achieved (Figure 5).
Figure 5: Coronary angiography after the final coil embolization Successful hemostasis was achieved.
After these embolization, CK and CKMB were slightly elevated (351 U/L and 44 U/L respectively), but no deterioration of cardiac function was observed. The patient has been followed up uneventfully at outpatient clinic for four months, on follow up CT examination; neither recurrence of bleeding nor enlargement of the hemopericardium was observed.
Discussion
This case suggested two important clinical issues. First of all, spontaneous coronary artery rupture (SCAR) can happen asymptomatically. Although SCAR is quite rare, all of the reported cases have sudden onsets and are critical ones [1-4]. However, our case presented silent progression and incidentally identified by the routine follow-up CT scan. He was hemodynamically stable and asymptomatic. Regardless of severe compression of the left ventricle by the hemopericardium, echocardiography did not show any deterioration of cardiac function. Furthermore, the hemopericardium was observed as spatial inhomogeneity of CT density. These findings suggest that the coronary bleeding was not in a continuous state and might explain the reason why the patient had been asymptomatic.
Second, 4D-CT is a useful diagnostic tool for identifying ruptured sites and coronary embolization is reasonable treatment for SCAR. 4D-CT is a dynamic volume imaging system of moving organs. It is beneficial for dynamic study of heart and perfusion study of vessels [5]. In this case, first session of catheterization did not reveal the extravasation from OM1. However 4D-CT was able to localize persistent extravasation from the artery. In addition, catheter embolization is efficient for SCAR. In the previously reported cases of SCAR, all of them were surgically treated. However if ruptured sites were identified by 4D-CT or CAG, coronary embolization as an option for hemostasis might be more practical because it is less invasive. As in this case, micro-coils and absorbable gelatin sponge particles have successfully stopped the bleedings.
In this case, final follow-up CT examination was performed four months after the second coil embolization. The relatively short follow-up period is one of the limitations of this case. Although CT examination still showed persistent hemopericardium, no further enlargement of the size was observed, suggesting that hemostasis was achieved. As the hemopericardium has been formed chronically and might be already organized and strongly adhered suggesting that it would be considered to remain there for a while and careful follow-up is needed.
As such a rare condition and there are few case reports of primary SCAR, it is quite difficult to establish any etiological pattern for the occurrence of SCAR. External rupture of atheromatous plaque ulcer and other coronary artery pathological factors such as aneurysm, and inflammatory processes or localized trauma should be taken into consideration as Shrestha et al. discussed [6].
Two cases of SCAR after the thoracic surgery have been reported [1,2], and all of them mentioned that they did not disturb the ruptured sites during the procedures. In this case as well, total arch replacement was performed as usual ways which means posterolateral wall of the heart was remained untouched. Of course, we could not exclude the possibility that disseminated intravascular coagulation (DIC) during the surgery and postoperative changes in hormones or inflammatory cytokines might have affected the coronary artery as Ozawa et al discussed [2]. However, earlier CT scan which was performed two weeks after the surgery showed pericardium without any extravasation meaning that the bleeding occurred during chronic phase. As CT and echocardiography were not performed thereafter, it is difficult to speculate when the rupture occurred.
Conclusion
In conclusion, SCAR can happen asymptomatically. In patients suspicious of SCAR, 4D-CT is efficient for identifying ruptured sites and coronary embolization is a feasible treatment. Although the relationship between SCAR and the surgery is unknown, careful follow up are needed after the thoracic surgery.
References
- Motoyoshi N, Komatsu T, Moizumi Y, et al. Spontaneous rupture of coronary artery. Eur J Cardiothorac Surg. 22: 470-471(2002).
- Ozawa Y, Ichimura H, Sato T, et al. Cardiac tamponade due to coronary artery rupture after pulmonary resection. Ann Thorac Surg. 96: e97-99 (2013).
- Butz T, Lamp B, Figura T, et al. Images in cardiovascular medicine. Pericardial effusion with beginning cardiac tamponade caused by a spontaneous coronary artery rupture. Circulation. 116: 383-384 (2007).
- Mayr B, Buchholz S, Hagl C, et al. Hemopericardium due to idiopathic coronary artery rupture treated with saphenous vein patch plasty. Thorac Cardiovasc Surg Rep.5: 54-56 (2016).
- Endo M, Tsunoo T, Kandatsu S, et al. Four-dimensional computed tomography (4D CT)--concepts and preliminary development. Radiat Med. 21: 17-22 (2003).
- Shrestha BM, Hamilton-Craig C, Platts D, et al. Spontaneous coronary artery rupture in a young patient: a rare diagnosis for cardiac tamponade. Interact Cardiovasc Thorac Surg. 9: 537-539 (2009).