Case Report - International Journal of Clinical Rheumatology (2020) Volume 15, Issue 6
Occipital neuralgia reavealing an atlantoaxial subluxation in an ankylosing spondylitis patient
- Corresponding Author:
- Rim Dhahri
1Department of Rheumatology
Military Hospital of Tunsi, Tunisia
E-mail: rimdhahri@ymail.com
Abstract
Occipital neuralgia is a peripheral neuropathy of the neck and head characterized by "unilateral paroxysmal headache of cervical origin", caused mostly by irritation or of the posterior large occipital nerve. We report the case of a patient with known history of axial and peripheral spondyloarthritis presenting with an unremitting right sided headache evolving for 2 months before examination. The Aetiological research revealed an atlantoaxial subluxation combining vertical and rotatory movements. The patient was surgically treated with C1/C2 laminectomy, an enlargement of the magnum canal and an occipito cervical arthrodesis reinforced posteriorly by a bone graft. While anterior atloaxoidal subluxation has been widely described in spondyloarthritis especially peripheral ones, vertical and rotatory subluxation has been rare to be seen especially when revealed by an occipital neuralgia.
Keywords
occipital neuralgia • spondyloarthritis • atlanto axial vertical subluxation • atlantoaxial rotatory dislocation
Case report
We report the case of a 33 year old man, with history of axial and peripheral spondyloarthritis. The diagnosis was retained five years ago on ACR Eular criteria : stage 3 sacroiliitis, talalgia, HLAB27 positive and oligoarthritis. The patient was initially treated with NSAIDs and Sulfasalazine with no subsequent improvement. He then received 3 courses of Infliximab switched by Etanercept. The patient progressed poorly with bilateral coxitis requiring the fitting of two total prostheses. Both knees were also damaged, and it was during his hospitalization for knee prosthesis that he described a right sided headache.
He has a spontaneous right unilateral posterior headache going from cervico-occipital junction ascending towards the homolateral temploral region. The pain was continuous, of a mixed nociceptive and neuropathic pattern with reported electric discharges. Nociceptive pain was scored by VAS scale to 7/10. Neuropathic pain was at 6 based on DN4 score. These symptoms evolved for two months before his hospitalization.
On examination, the cervical spine was stiff, limited in extension-flexion, inclinations and rotations. Deep tendon reflexes were normal as well as the rest of the neurological examination apart from paraesthesia in the sensitive territory of the right great occipital nerve. The unidigital pressure at the cervico-occipital junction reproduced the pain: Trigger zone. The patient was put on analgesics and Pregabalin at a dose of 150 mg/day without great efficacy.
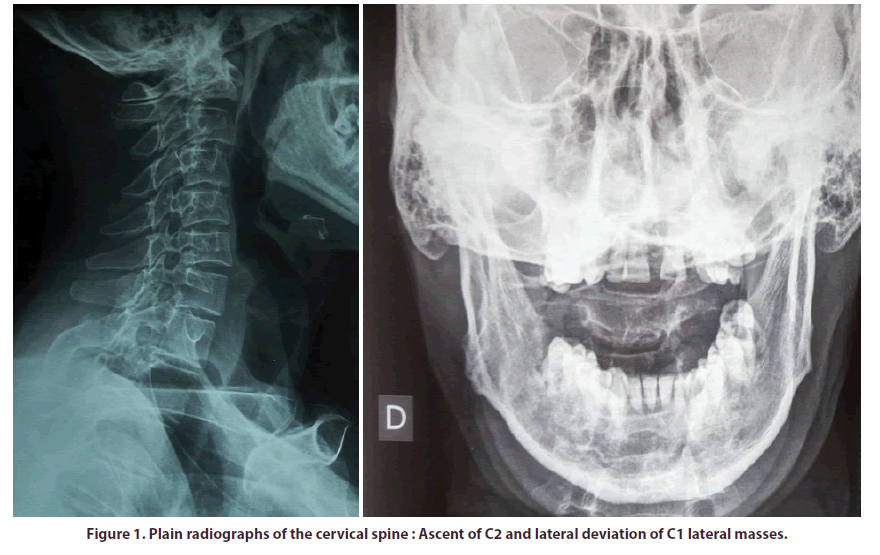
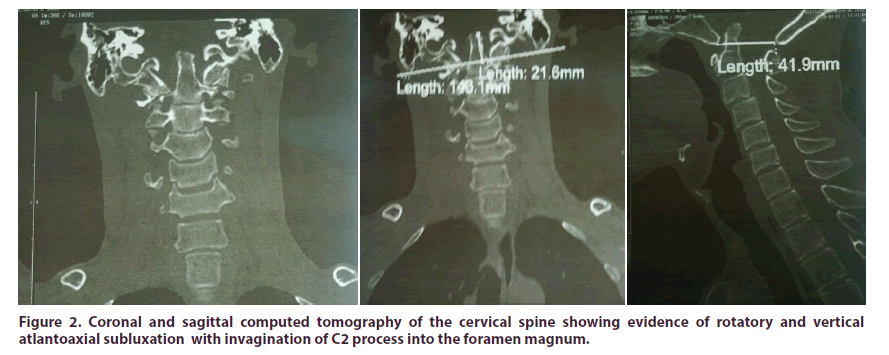
Due to the unremitting nature of our patient’s symptoms a plane radiographs of the cervical spine were requested. They showed an ascent of the odontoid process (Figure 1) along with a lateral deviation of C1 masses. MRI and CT scann (Figures 2 & 3) confirmed the rotary and vertical atloaxoidal subluxation. They showed a Type I atlantoaxial rotatory dislocation according to Fielding and Hawkins classification of Atlantoaxial Rotatory Subluxation (AARS) [1]. Morover, they showed an invagination of the odontoid process in cranial space exceeding the bi mastoid line of 22 mm and compressing the medullary junction with no signs of myelomalacia. The patient was treated with a sternaloccipital- mandibular immobilizer. Surgical treatment was retained based on the persistance of symptoms and important complications’ risk.
Figure 2: Coronal and sagittal computed tomography of the cervical spine showing evidence of rotatory and vertical atlantoaxial subluxation with invagination of C2 process into the foramen magnum.
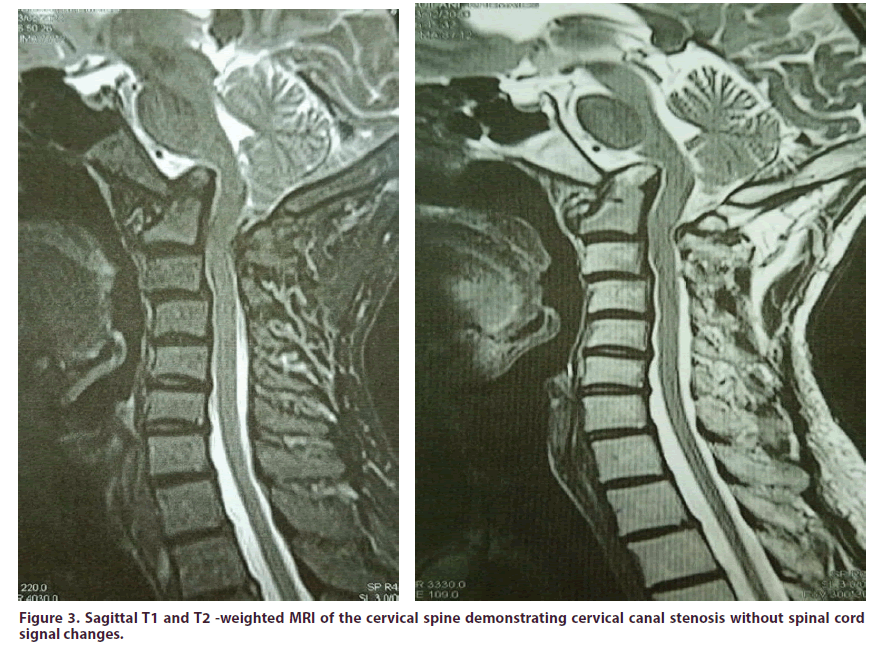
Figure 3: Sagittal T1 and T2 -weighted MRI of the cervical spine demonstrating cervical canal stenosis without spinal cord signal changes.
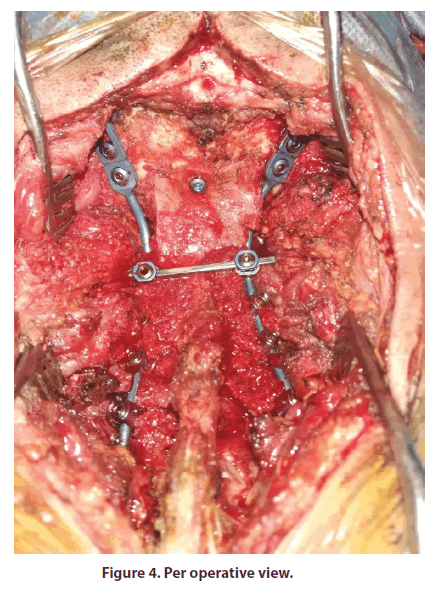
The surgical management consisted in a C1 laminectomy relieving the cervical cord which was compressed at this level, an enlargement of the foramen magnum and in a cervical occipito arthrodesis (occiput - C4 / 5/6), reinforced posteriorly by a bone graft (Figure 4).
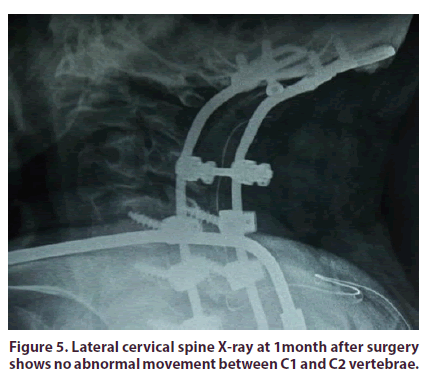
The post-operative course was favorable. At two weeks after surgery, our patient was restarted on celecoxib and Sulfasalazine. Pain scales dropped significantly (VAS at 3/10 and DN4 at 2). Lateral cervical spine X-ray with flexion view at one month after surgery showed no abnormal movement between C1 and C2 vertebrae (Figure 5).
Figure 5: Lateral cervical spine X-ray at 1month after surgery shows no abnormal movement between C1 and C2 vertebrae.
Discussion
This report highlits the fact that upper cervical spine have to be assessed carefully in AS patients, especially when clinical signs such as occipital neuralgia occurs. It raises also the fact that atlantoaxoidal subluxation is not always anterior and may be more complex with vertical and rotatory dislocations. Discrepancies between clinical and imaging findings are also to be taken into caccount.
Ankylosing Spondylitis (AS) is, in fact, a chronic inflammatory, condition that involves axial and peripheral joints. Untreated, it usually progresses towards stiffness of the spine. Cervical spine may be involved in late stages of the disease [2].
Cervicel subluxation is although less frequently described than in other rheumatic conditions such as Rheumatoid Arthritis (RA) [3,4] with a prevalence of 12% and even up to 86% in some reports. The atloaxoidal dislocation is mostly anterior with 2%-6.7% and up to 21% in AS. Vertical subluxation is more rare up to 2%in AS [4] compared to 5 to 34% of patients with RA [5]. It has been defined as the ascent of the odontoid process above McRae’s foramen magnum line (opisthionexion) [2]. In some reports ,there was a relative paucity of specific neurological signs despite the impressive cervicomedullary compression usually seen on MRI.
Rotatory subluxation is mostly seen in paediatric patients with conditions that predispose them to ligamentous laxity. It has rarely been described in adults and is usually associated with trauma. Few cases associated with spondyloarthritis have been described in literature: two children with undifferentiated forms and two young adults with Ankylosing Spondylitis (AS) [6,7].
Although most patients remain asymptomatic in AS as well as in RA, about 32% show radiologic progression during followup [8,9]. A strict evaluation is crucial because AAS may lead to spinal cord compression, vascular compression, and other complications which requires intervention at an early stage.
Risk factors for subluxation in AS are a longer duration of AS and the presence of peripheral arthritis, while risk factors reported for rheumatoid AAS include a later onset of RA (age>45 yrs), active synovitis, rapidly progressive erosive peripheral arthritis, and rheumatoid factor . However, the prevalence and risk factors vary depending on study subjects, and have limitations due to small study size [8].
Duration of disease has been recognized as a major factor that determines cervical spine involvement, including AAS in AS and spondyloarthropathy. Peripheral arthritis was also reported as a risk factor for cervical spine diseases in psoriatic spondylitis, and AAS occurred in up to two-thirds of cases that had persistent peripheral arthritis [10]. Cervical spine X-rays and CT examination are essential. MRI may show proliferation of the synovium (pannus formation), myelomalacia, and cervical canal stenosis.
Indications for surgical intervention include: symptoms and signs of cervical myelopathy, intractable mechanical occipitocervical neck pain, worsening of atlantoaxial instability), previous MRI evidence of spinal cord injury (myelomalacia), and MRI evidence of persistent active inflammation despite immunomodulating medical therapy [11].
Conclusion
Occipital Neuralgia (ON) is a cervicogenic headache originating mostly from the great occipital nerve compression. Its occurrence should lead the practicionar to suspecting an upper cervical injury. Alantoaxial subluxation is a rare cause of ON. Spontaneous subluxation itself is an uncommon complication of spondyloarthritis. Several clinical features are to be highlited in order to recognize at an early stage this complication:long term evolving disease and peripheral arthritis. Close follow-up is mandatory for these patients.
Funding
None.
Conflict of interest
None to declare.
Ethics
The pateint was informed and fully consents to publication.
References
- Ciftdemir M, Copuroğlu C, Ozcan M et al. Non-operative treatment in children and adolescents with atlantoaxial rotatory subluxation. Balk. Med. J. 29(3), 277–280 (2012).
- Archer JR, Keat AC. Ankylosing spondylitis: time to focus on ankylosis. J. Rheumatol. 26(4), 761–764 (1999).
- Nguyen HV, Ludwig SC, Silber J et al. Rheumatoid arthritis of the cervical spine. Spine. J. Off. J. North. Am. Spine. Soc. 4(3), 329–334 (2004).
- Ramos-Remus C, Gomez-Vargas A, Guzman-Guzman JL et al. Frequency of atlantoaxial subluxation and neurologic involvement in patients with ankylosing spondylitis. J. Rheumatol. 22(11), 2120–2125 (1995).
- Casey AT, Crockard HA, Geddes JF et al. Vertical translocation: the enigma of the disappearing atlantodens interval in patients with myelopathy and rheumatoid arthritis. Part I. Clinical, radiological, and neuropathological features. J. Neurosurg. 87(6), 856–862 (1997).
- Muscal E, Satyan KB, Jea A. Atlantoaxial subluxation as an early manifestation in an adolescent with undifferentiated spondyloarthritis: a case report and review of the literature. J. Med. Case. Rep. 5(1), 275 (2011).
- Chien JT, Chen IH, Lin KH. Atlantoaxial rotatory dislocation with hypoglossal nerve palsy in a patient with ankylosing spondylitis. A case report. J. Bone. Joint. Surg. Am. 87(7), 1587–1590 (2005).
- Lee JS, Lee S, Bang SY et al. Prevalence and risk factors of anterior atlantoaxial subluxation in ankylosing spondylitis. J. Rheumatol. 39(12), 2321–2326 (2012).
- Ramos-Remus C, Gomez-Vargas A, Hernandez-Chavez A et al. Two year followup of anterior and vertical atlantoaxial subluxation in ankylosing spondylitis. J. Rheumatol. 24(3), 507–510 (1997).
- Sallés M, Clavaguera T, Mínguez S et al. Atlantoaxial rotatory dislocation in a patient with psoriatic spondyloarthritis. Joint. Bone. Spine. 86(4), 519–521 (2019).
- Wu X, Wood KB, Gao Y et al. Surgical strategies for the treatment of os odontoideum with atlantoaxial dislocation. J. Neurosurg. Spine. 28(2), 131–139 (2018).