Case Report - Interventional Cardiology (2018) Volume 10, Issue 6
Feasibility, safety and efficacy of peripheral arteriographies through radial access. Early clinical experience of 40 consecutive cases
- Corresponding Author:
- Ricardo de Souza A.
Ferreira
HCI - Santa Casa de Misecórdia de São Sebastião do Paraíso – Hospital Regional do Coração do Sul de Minas Gerais, São Sebastião do Paraíso, MG, Brasil
Tel: 09008740965
Fax: 416-603-6919
E-mail: Arina.Bingeliene@uhn.ca
Received date: June 17, 2018 Accepted date: October 01, 2018 Published date: October 08, 2018
Abstract
Introduction: Transradial approach (TRA) is a well-established technique for settings of coronary intervention, showing superiority above transfemoral approach (TFA). Most of the benefits of TRA approach can be reproduced to peripheral vascular approaches, despite the absence of scientific evidences in this setting. TRA access has been gradually emerging as an alternative and effective way for arteriographies and vascular interventions comparing to TFA. Our objective is to demonstrate the feasibility and safety of TRA access for the accomplishment of peripheral arteriographies and to provide a guide for those who look for a new TRA peripheral program.
Method: series of 40 consecutive cases, with description of the technique, complications and immediate and short term results of peripheral and visceral arteriographies through TRA access in Hospital Regional do Coração , in the South of Minas Gerais.
Results: Between August, 2017 and March, 2018, 40 patients were submitted to peripheral and visceral arteriographies through TRA access. All the procedures were performed and ended through radial access, with only one crossover access, performed through contralateral radial artery. There were no major complications (bleeding, pseudoaneurysm, occlusion of the symptomatic radial artery, EASY>III hematoma, arteriovenous fistula). Seven patients presented EASY I hematoma, 85,71% female, 72 years of age, on average, and in a 100% of the cases the introducer was 6fr.
Conclusion: Peripheral and visceral arteriography through TRA access proved to be a safe and effective alternative. It allows precocious walking with low rates of complications.
Keywords
Radial access, Radial artery, Transradial approach, Peripheral arteriography, Peripheral arterial disease
Introduction
The increasing number of diagnosis and peripheral vascular interventions, raise the search of more safe and effective alternatives for diagnostic examinations and percutaneous treatment. Due to the high risk clinical profile of this population, the use of endovascular techniques can offer broader benefit, especially when associated to safer strategies of arterial access. Information from literature related to coronary disease show significant decrease in terms of vascular complications and/or bleedings in the access area, when the approach is performed through TRA access, compared to TFA traditional access [1-3].
Most of the vascular complications seen with TFA access, like bleeding in puncture area, pseudoaneurysms, arteriovenous fistulas and member ischaemia are significantly lower with TRA approach [1,2,4]. This is probably due to single anatomical characterists of RA, including its easy compression, relative isolation of surrounding veins and double irrigation of palmar arch.
Intuitively the diagnostic procedures and percutaneous peripheral interventions through radial access may bring benefits to the patients, mostly in relation to vascular complications and bleeding, although this fact has not been proved yet in randomized clinical trial.
In this manuscript, an early initial experience of 40 consecutive cases of peripheral or visceral arteriographies through TRA access is described, evaluating its feasibility, efficacy and safety and discussing technical aspects of the procedure.
Methods
A series of 40 cases of peripheral and visceral arteriographies held through TRA access. All the cases were accomplished at Hospital Regional do Coração, in the south of Minas Gerais. The selection of patients involved the assessment of enabling anatomical conditions for the TRA approach, with the execution of Allen [5] and/or Barbeau [6] tests. The eligible patients were advised about the risks and benefits of the procedure and all of them, voluntarily and well aware, signed the term of agreement.
Criterion for inclusion:
Eligible patients for peripheral arteriography, abdominal aortography and visceral arteriography.
Criterion for exclusion:
Patients with contraindications for radial access.
Study population
All the patients directed to diagnostic peripheral arteriography, abdominal aortography and visceral arteriography were examined prospectively, in the period between August, 2017 and March 2018, in an only center. All the operators were familiarized with radial access for angiographies or percutaneous coronary interventions.
Procedures
The radial artery was punctured with Jelco 20- 22 catheter through Seldinger or modified Seldinger technique, using a 5 or 6 Fr hydrophilic short sheath introducer. A solution containing 5.000 UI of non-fractioned heparin and 10mg of isosorbide mononitrate was administered through the extent of sheath. 5 or 6 Fr Multipurpose or 125cm PigTail catheters (Merit Medical, South Jordan, UT, and USA) were used. When it was technically difficult to cross the aortic arch, specific techniques were used, like deep inspiration, guide wire loop in ascending aorta, curved guide wire catheter (JudkinsLeft, PigTail, Amplatzer), hydrophilic and/or extra stiff swap guide (260-300cm).
When the procedure was finished, the sheath introducer was immediately removed, and hemostasis with compression dressing was done. Patients were authorized for walking after 10 minutes.
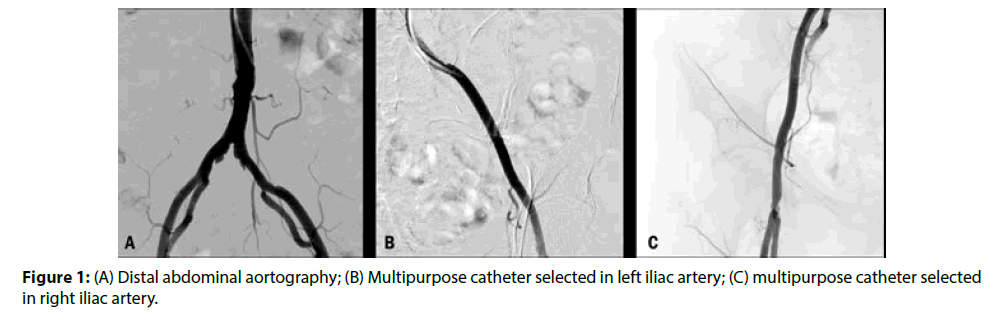
The arteriography was carried with the help of injection pump or manual injection, with the choice of the target artery and sequential angiographies until distal segments (Figure 1).
Eligible patients were discharged after 2 h in observation.
Endpoints of interest and definitions
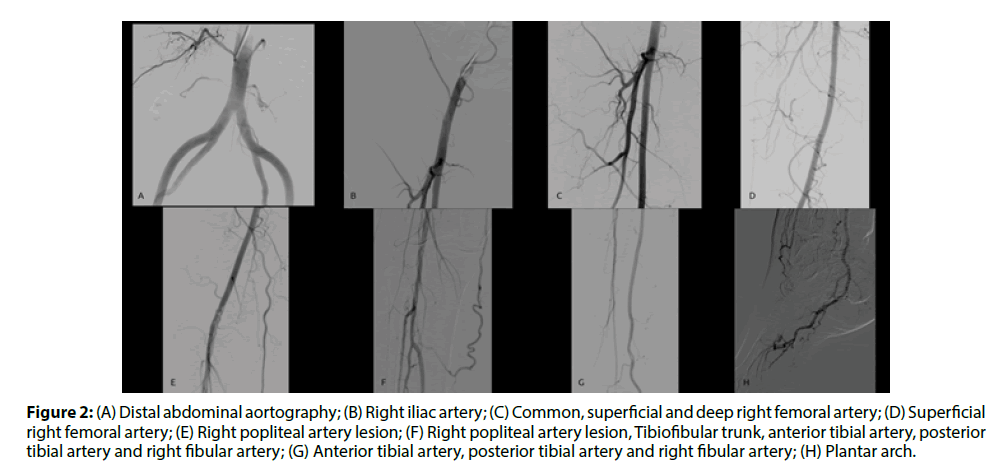
The efficacy of the technique was evaluated through the success rate of the procedure, defined as full implementation of arteriography, without the necessity of changing the access. The length of the procedure and the fluoroscopy time were obtained from the beginning of the passage of the guide wire in radial artery until the removal of the catheter (Figure 2).
Figure 2: (A) Distal abdominal aortography; (B) Right iliac artery; (C) Common, superficial and deep right femoral artery; (D) Superficial right femoral artery; (E) Right popliteal artery lesion; (F) Right popliteal artery lesion, Tibiofibular trunk, anterior tibial artery, posterior tibial artery and right fibular artery; (G) Anterior tibial artery, posterior tibial artery and right fibular artery; (H) Plantar arch.
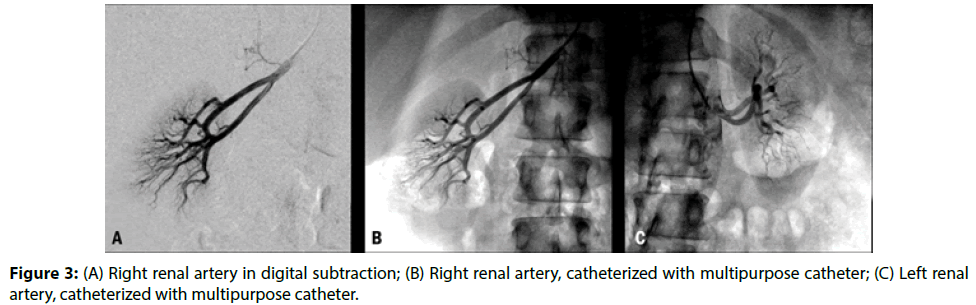
The safety was evaluated through the occurrence of vascular complications related to the puncture place, including acute bleeding, hematoma, arteriovenous fistula, pseudoaneurysm, symptomatic arterial occlusion or necessity of repairing vascular surgery. Hematoma was evaluated according to EASY (Early Discharge after Transradial Stenting of Coronary Arteries) [7] classification. Peripheral arterial disease was evaluated according to Rutherford [8] classification (Figure 3).
Patients were evaluated two hours after the end of the procedure and through questionnaire thirty days after the procedure.
Statistical analysis
Qualitative variables were summarized in absolute frequencies and percentages, and quantitative analysis was described as medium±pattern deviation.
Results
In total, 40 patients with indication for peripheral or visceral arteriography were selected to TRA approach. Basal clinical characteristics are described in the Table 1. Among the patients, 55% male and 45% female, 62 years of age, on average. Tobacco use and systemic hypertension were the risk factors with greater prevalence, 85% and 77% respectively. In all the patients the realization was possible through radial access, 38 patients through right radial access and 2 patients through left radial access. The initial choice was according to the operator. In one patient it was necessary to remove the crossover access, due to tortuosity of the aortic arch and the failure to cross it even with the use of specific techniques, and it was accomplished through contralateral radial access (left radial). 36 arteriographies of lower limbs, 3 abdominal aortographies and 1 renal arteriography were accomplished. Information about the procedures is described in Table 2. There were no major complications (bleeding, pseudoanurysm, symptomatic radial artery occlusion, EASY hematoma III, arteriovenous fistula). Two hours after the procedure, 7 of the patients presented hematomas classified as EASY I, among them, 6 (85.71%) were female and in all the cases the introducer used was 6Fr. Data relating to patients that presented hematomas is demonstrated in Table 3. In the evaluation after 30 days, none of the patients presented symptomatic complications related to vascular access.
| Variables | General n (% ou SD) |
|---|---|
| Male sex, n (%) | 22 (55) |
| Female sex, n (%) | 18 (45) |
| Age, years | 62 (± 13) |
| BMI, (kg/m2) | |
| Undernutrition, n (%) | 1 (2,5) |
| Eutrophia, n (%) | 18 (45) |
| Overweight, n (%) | 16 (40) |
| Obesity, n (%) | 5 (12,5) |
| Systemic hypertension, n (%) | 31 (77,5) |
| Diabetes mellitus, n (%) | 14 (35) |
| Systemic hypertension, n (%) | 31 (77,5) |
| Diabetes mellitus, n (%) | 14 (35) |
| Dyslipidemia, n (%) | 29 (72,5) |
| Tobacco use, n (%) | 34 (85) |
| Chronic renal failure RRT, n (%) | 1 (2,5) |
| Rutherford classification, n (%) | 38 (95) |
| Category II, n (%) | 3 (8) |
| Category III, n (%) | 9 (24) |
| Category IV, n (%) | 10 (26) |
| Category V, n (%) | 16 (42) |
| Subtitle: SD, standard deviation; BMI: body mass index; RRT: renal replacement therapy. | |
Table 1: Basal Clinical Characteristics
| Variables | General n (% ou SD) |
|---|---|
| Lower limbs arteriography, n (%) | 36 (90) |
| Abdominal aortography, n (%) | 3 (7,5) |
| Renal arteriography, n (%) | 1 (2,5) |
| Introducer sheath | |
| 5FR, n (%) | 16 (40) |
| 6FR, n (%) | 24 (60) |
| Diagnostic catheter | |
| Multipurpose, n (%) | 29 (72,5) |
| Pigtail, n (%) | 11 (27,5) |
| Access | |
| Left radial, n (%) | 2 (5) |
| Right radial, n (%) | 38 (95) |
| Crossover access*, n (%) | 1 (2,5) |
| Fluoroscopy time, minutes (±SD) | 14,73 (± 6,53) |
| Hematoma | |
| EASY (I), n (%) | 7 (18) |
| Subtitle: SD, standard deviation; *Crossover from right radial to left radial. No bleeding; FR, French. | |
Table 2: Characteristics of the procedure
| Variables |
General n (% ou SD) |
|---|---|
| Hematoma | |
| EASY (I), n (%) | 7 (18) |
| Woman, n (%) | 6 (85,71) |
| Men, n (%) | 1 (14,29) |
| Age, years | 72 (±9) |
| BMI (Kg/m2) | |
| Undernutrition, n (%) | 1 (14,29) |
| Eutrophya, n (%) | 3 (42,86) |
| Overweight, n (%) | 2 (28,56) |
| Obesity, n (%) | 1 (14,29) |
| Hypertension, n (%) | 6 (85,71) |
| Tobacco use, n (%) | 6 (85,71) |
| Diabetes Mellitus, n (%) | 3 (42,86) |
| Insulin-dependent, n (%) | 2 (28,56) |
| Non insulin-dependent, n (%) | 1 (14,29) |
| Chronic renal failure RRT, n (%) | 1 (14,29) |
| Introducer sheath6FR, n (%) | 7 (100) |
| Subtitle: SD, standard deviation; BMI, body mass index; RRT, renal replacement therapy; FR, French. | |
Table 3: Predictores for hematoma
Discussion
Transradial (TRA) approach for angiography and coronary interventions is a well-established technique [2,9,10]. Campeau described for the first time the use of radial artery access for coronary angiography in 1989 [11,13]. After that, Kiemeneij and Laarman performed the first coronary intervention using this approach in 1993. 12 It showed its superiority above transfemoral (TFA) approach and transbrachial (TBA) approach to set itself as an effective alternative technique for most of the situations of coronary intervention [2,9,10]. Most of the benefits of TRA approach can be reproduced to peripheral vascular approaches, despite the absence of scientific evidences in this setting. Some observational studies, feasibility studies, technical reports, series of cases and case reports demonstrated the successful application of this technique to deal with peripheral vascular injuries, including internal, vertebral and basic, subclavian, innominate, renal, iliac, celiac, mesenteric and superficial carotid of femoral artery [1,9,14]. TRA access is gradually emerging as an effective and alternative access for arteriographies and vascular interventions comparing to TFA. It is associated with fewer vascular complications compared with femoral access [15-17]. The meta-analysis 15,18 of randomized controlled trials comparing radial versus femoral access for primary percutaneous coronary interventions (PCIs) revealed that the radial approach was significantly associated with increased risk of major bleeding (1.4% vs. 2.9%) and access site bleeding (2.1% vs. 5.6%). Scant data are available regarding the use of this alternative approach in peripheral vascular diseases [15,19,20], the largest amount of prospective data on access to complications from the coronary literature [15-17]. In the prospective multicenter RIVAL (Radial vs. Femoral Access for Coronary Angiography and Intervention in Patients with Acute Coronary Syndromes) study [15,17] rates of major vascular complications (large hematomas, pseudoaneurysm needing closure, arteriovenous fistula) and minor bleeding with femoral access were 3.7% and 3.4%, respectively. Another issue with femoral access is the need for patients to stay supine several hours after the procedure [15,21,22]. In the current era, the femoral artery is considered to be the first-choice access site for percutaneous peripheral approach. Although this approach is usually simple and fast to perform, several issues remain. The femoral artery can be hard to puncture, even when using duplex scan guidance, especially in the setting of obese patients or antegrade access [15,23]. In some cases, femoral artery puncture can be considered at increased risk of local complications or failure, such as in the absence of palpable femoral pulses, the presence of common femoral artery calcifications, obesity, a history of femoral surgery (especially with prosthetic materials), or the need for a contralateral femoral approach. Moreover, postoperative hematomas account for significant postoperative morbidity [15,23,24]. The technique of radial puncture has some inconvenient, though. First of all, radial artery presents a relative risk of vasospasm mediated by puncture, and it is required a learning curve with the access for the operators of little or no experience with this vascular access. Another important point is in relation to the aortic arch crossing which, sometimes, is not technically simple, and the use of specific techniques is necessary, like deep inspiration, guide wire loop in ascending aorta, use of curved guide catheter (JudkinsLeft, PigTail, Amplatzer), use of hydrophilic and/or extra hard swap guide (260-300 cm). Finally, the short length of a typical radial catheter is an important disadvantage for the technique, as the use of longer catheters (125 cm) is required, due to the longer way to be crossed until the target artery for the angiography. However, the development of devices dedicated to transradial peripheral, diagnostic and therapeutic procedures should facilitate the use of the technique in the future. In our experience, the routine use of radial access in peripheral and visceral arteriographies proved to be feasible, according to the high rate of success of the procedure and the low rate of crossover. Thus, the efficacy and safety profile associated to the radial access in the accomplishment of peripheral and visceral arteriographies makes its choice recommended, since it is accomplished by qualified operators, familiarized with its usage, especially those who elected the technique as their first option, supplanting in this way the learning curve and eventual technical difficulties, allowing the accomplishment of an invasive exam that allows the patient precocious walking, greater comfort e lower rates of vascular complications related to the puncture place.
Study Limitations
This study presents obvious limitations due to its descriptive aspect and without the presence of control group, with non-random nature, short term monitoring and small population of patients.
Conclusion
TRA Access provides a safe and alternative access in relation to TFA for peripheral and visceral arteriographies. Its application allows discharge and precocious walking, greater satisfaction for the patient and less local bleeding complications. The left radial artery can facilitate since it avoids the necessity to cross the aortic arch, although the right radial artery is more comfortable to the operator and it presents high rates of success. TRA approach offers advantages and should be considered for routine peripheral arteriography.
Conflicting Interests
None
Source of Funds
None
References
- Staniloae CS, Korabathina R, Coppola JT. Transradial access for peripheral vascular interventions. Catheter Cardiovasc Interv. 81(7): 1194-1203 (2013).
- Agostoni P, Biondi-Zoccai GG, de Benedictis ML, et al. Radial versus femoral approach for percutaneous coronary diagnostic and interventional procedures: systematic overview and meta-analysis of randomized trials. J Am Coll Cardiol. 44: 349-356 (2004).
- Jolly SS, Amlani S, Hamon M, et al. Radial versus femoral access for coronary angiography or intervention and the impact on major bleeding and ischemic events: A systematic review and meta-analysis of randomized trials. Am Heart J. 157: 132–140 (2004)
- Jolly SS, Yusuf S, Cairns J, et al. Radial versus femoral access for coronary angiography and intervention in patients with acute coronary syndromes (RIVAL): A randomised, parallel group, multicentre trial. Lancet. 377: 1409-1420 (2011).
- Allen EV. Thromboangiitis obliterans: methods of diagnosis of chronic occlusive arterial lesions distal to the wrist with illustrative cases. Am J Med Sci. 178(2): 237-44 (1929).
- Barbeau GR, Arsenault F, Dugas L, et al. Evaluation of the ulnopalmar arterial arches with pulse oximetry and plethysmography: comparison with the Allen´s test in 1010 patients. Am Heart J. 147(3): 489-93 (2004).
- Bertrand OF, Larose E, Rodes-Cabau J, et al. Incidence, predictors, and clinical impact of bleeding after transradial coronary stenting and maximal antiplatelet therapy. Am Heart J. 157(1): 164-169 (2009).
- Rutherford RB, Baker JD, Ernst C, et al. Recommended standards for reports dealing with lower extremity ischemia: revised version. J Vasc Surg. 26: 517-38 (1997).
- Rutherford RB, Baker JD, Ernst C, et al. Utility of Transradial Approach for Peripheral Vascular Interventions. J Invasive Cardiol. 27(6): 277-282 (2015).
- Kiemeneij F, Laarman GJ, Odekerken D, et al. A randomized comparison of percutaneous transluminal coronary angioplasty by the radial, brachial and femoral approaches: the ACCESS study. J Am Coll Cardiol. 29: 1269-1275 (1997).
- Campeau L. Percutaneous radial artery approach for coronary angiography. Cathet Cardiovasc Diagn. 16: 3-7 (1989).
- Kiemeneij F, Laarman GJ. Percutaneous transradial artery approach for coronary stent implantation. Cathet Cardiovasc Diagn. 30: 173-178 (1993).
- Coppola JT, Cezar Staniloae. Radial Access for Peripheral Vascular Procedures. Endovasc Today. 38-44 (2012).
- Sanghvi K, Kurian D, Coppola J. Transradial intervention of iliac and superficial femoral artery disease is feasible. J Interv Cardiol. 2: 385-387 (2008).
- Coscas R, Blic R, Capdevila C, et al. Radial access for peripheral transluminal angioplasty. J Vasc Surg. 61: 463-468 (2015).
- Baklanov DV, Kaltenbach LA, Marso SP, et al. The prevalence and outcomes of transradial percutaneous coronary intervention for ST-segment elevation myocardial infarction: analysis from the National Cardiovascular Data Registry (2007 to 2011). J Am Coll Cardiol. 61: 420-6 (2013).
- Jolly SS, Yusuf S, Cairns J, et al. RIVAL trial group. Radial versus femoral access for coronary angiography and intervention in patients with acute coronary syndromes (RIVAL): a randomised, parallel group, multicentre trial. Lancet. 377: 1409-1420 (2011).
- Karrowni W, Vyas A, Giacomino B, et al. Radial versus femoral access for primary percutaneous interventions in ST-segment elevation myocardial infarction patients: a meta-analysis of randomized controlled trials. JACC Cardiovasc Interv. 6: 814-23 (2013).
- Trani C, Tommasino A, Burzotta F. Pushing the limits forward: transradial superficial femoral artery stenting. Catheter Cardiovasc Interv. 76: 1065-1071 (2010).
- Sanghvi K, Kurian D, Coppola J. Transradial intervention of iliac and superficial femoral artery disease is feasible. J Interv Cardiol. 21: 385-397 (2008).
- Akopian G, Katz SG. Peripheral angioplasty with same-day discharge in patients with intermittent claudication. J Vasc Surg. 44: 115-118 (2006).
- Gouicem D, Palcau L, Le Hello C, et al. Feasibility of ambulatory percutaneous femoral access without the use of arterial closure systems. Ann Vasc Surg. 28: 132-136 (2014).
- Wheatley BJ, Mansour MA, Grossman PM, et al. Complication rates for percutaneous lower extremity arterial antegrade access. Arch Surg. 146: 432-435 (2011).
- Dick P, Barth B, Mlekusch W, et al. Complications after peripheral vascular interventions in octogenarians. J Endovasc Ther. 15: 383-389 (2008).