Case Report - Interventional Cardiology (2018) Volume 10, Issue 5
2 cases of non-surgical treatment of stent loss during percutaneous coronary intervention
- Corresponding Author:
- Mohamed Aymen Ben
Abdessalem
Centre Hospitalier Universitaire Farhat Hached de Sousse sousse, sousse Tunisia
Tel: +21655820485
E-mail: x3azrael@yahoo.co.kr
Received date: July 30, 2018 Accepted date: September 26, 2018 Published date: October 05, 2018
Abstract
Background: Percutaneous coronary intervention with stents is widely used for coronary artery disease. Stent loss is a rare complication. Incidence is estimated at 1.3%. Although Stent has been retrieved in most cases; urgent coronary artery bypass graft, myocardial infarction and death are poor outcomes associated with this complication. Cases report: First case is about a 55 years old male, heavy smoker, admitted to the cathlab for a non ST elevation myocardial infarction (NSTEMI). Ejection fraction (EF) was 55% with inferior wall hypokinesis. Coronary angiogram showed a long stenosis in a tortuous mid-right coronary artery (RCA) with a TIMI 2 flow. Ad-hoc angioplasty was attempted. Direct stenting was attempted but stent couldn't be delivered to the target lesion and attempts resulted in stent retention. Stent couldn't be retrieved and finally was successfully crushed with a drug eluting stent with good final result. Patient had uneventful recovery. Second case is about a 59 years old Male type 2 diabetes mellitus and former smoker. He was hospitalized for a NSTEMI. EF was 50% with anterior hypokinesis. Angiogram showed a long stenosis in the mid left anterior descending artery with a TIMI 2 flow. Ad-hoc angioplasty was attempted with a long drug eluting stent (DES) but wasn't successful. The stent was partially detached and deformed. It was successfully retrieved using the stent's balloon. Patient was successfully treated with a second successful procedure with a DES. Conclusion: No algorithm or stepwise approach exists to treat stent loss. Tortuous lesions and failure to cross the stenosis are common angiographic finding associated with this complication. Stent retrieval, deployment or crushing is the frequently used techniques to deal with this issue.
Keywords
Cardiology, Interventionnal cardiology, Complication and Stent dislogement
Background and aims
Percutaneous coronary intervention (PCI) with stents is widely used for coronary artery disease (CAD). Stent loss is a rare complication. Incidence is estimated at 1.3% over the 3 past decades and has been decreasing with the improvement of stents delivery systems [1]. Although Stent has been retrieved in most cases; urgent coronary artery bypass graft, myocardial infarction and death are poor outcomes associated with this complication. Data concerning this complication is still sparse and no codified treatment exists. We hereby describe 2 cases of stents loss managed differently.
Cases Report
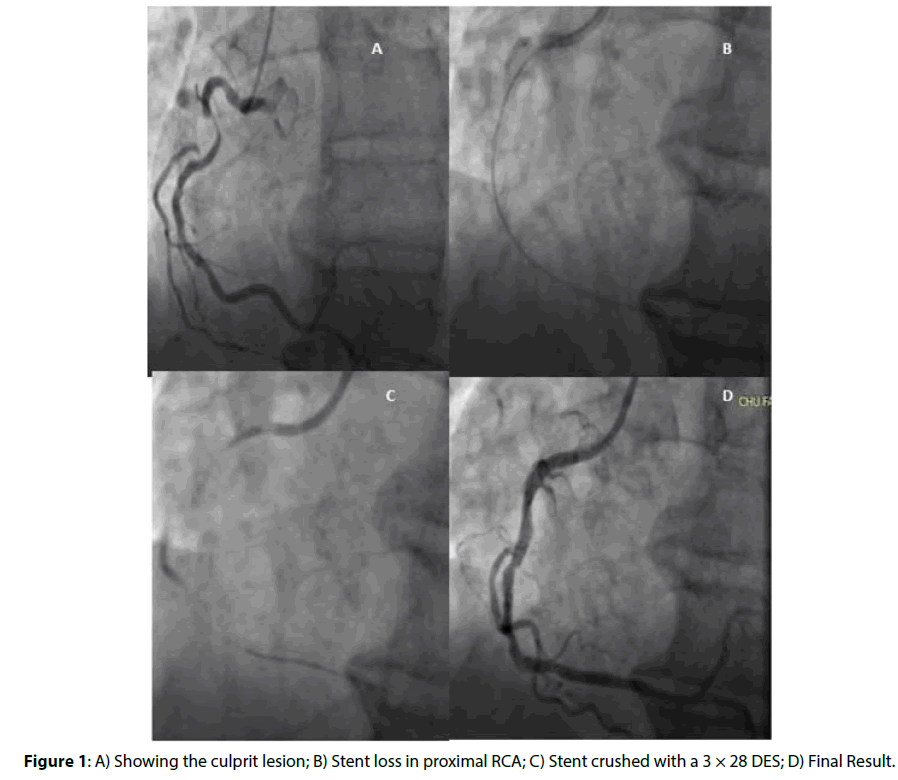
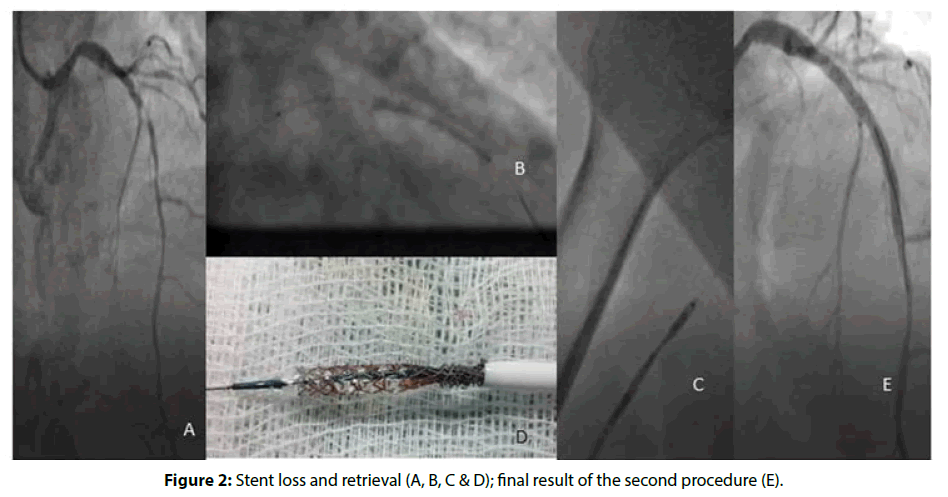
First patient is a 55 years old male, heavy smoker, admitted to the cathlab for a non ST elevation myocardial infarction (NSTEMI). Ejection fraction (EF) was 55% with inferior wall hypokinesis. Coronary angiogram, through radial access, showed a long stenosis in a tortuous mid-right coronary artery (RCA) segment; with a TIMI 2 flow (Figure 1A) and moderate disease in the remaining coronary arteries. Ad-hoc angioplasty was attempted. A 6Fr Judkins right 4 (Medtronic®, USA) guiding catheter was used to advance the guide wire through the lesion. A predilation with 2.5 × 10 mm Hiryu™ (Terumo®, Japan) was performed leaving a 50% residual stenosis. Stenting was attempted with a 3.0 × 12 mm Avantgarde™ bare metal carbo-stent (CID®,Italy) but stent couldn’t be delivered to the target lesion. We decided to withdraw it and do further balloon predilation but a resistance was perceived and attempts resulted in retention of the unexpanded stent in proximal RCA (Figure 1B) with guidewire in situ. No retrieval device was available. Expansion of the stent with small balloon 1.25 × 10 mm Ryujin™ (Terumo®, Japan) failed. Finally, a second guidewire was introduced in the RCA the noncompliant balloon was reused to crush and fix the stent. Then a 3.0 × 32 DESyne™ (Elixir®, USA) stent was deployed over the crushed stent. A TIMI 3 flow was achieved (Figures 1C and 1D). Patient had uneventful recovery. Second case: A 59 years old Male type 2 diabetes mellitus and former smoker was admitted for a NSTEMI. EF was 50 % with anterior hypokinesis. Coronary angiogram through radial access showed a long stenosis in the mid left anterior descending artery with a TIMI 2 flow (Figure 2A) with moderate disease in a dominant RCA. Ad-hoc angioplasty was attempted. A 6Fr Judkins left (Medtronic®, USA) was used to advance a guide wire through the lesion. After a pre-dilation with a 2.0 × 20 mm River™ (Balton®), a 2.75 × 38 mm DESyne™ (Elixir, USA) drug eluting stent was introduced but crossing the lesion wasn’t successful. A stent deformation was noticed and while withdrawing the stent it became partially separated from the balloon (Figure 2B). A 4 ATM inflation of the stent’s balloon was performed and the withdrawal of the stent within the guiding catheter and the sheath was achieved (Figures 2C and 2D). A second procedure through the same radial artery access was done with a 6Fr Extra back-up guiding catheter (Medtronic®, USA) and was successful. A 3.0 × 38 mm Promus™ (Boston scientific, USA) DES was used (Figure 2E).
Discussion
In our series the stent, partially dislodged, was retrieved in the second case without using a retrieval device. It was compressed at the site of the complication and fixed in the first case.
Coronary stent loss (CSL) is not exceptional, but a rare complication of PCI. A recent meta-analysis of 71 655 procedures over 3 decades from 1991 to 2012, recorded 919 cases of stent loss. The overall estimated frequency was 1.3% (95% CI [0.8%-2.8%]). This rate decreased from 5% before 1995 to 0.3% after 2005 [1]. Although factory crimped stents are the gold standard, this complication didn’t disappear completely. Recent case series describing this complication are still published [2-5].
Mechanism of stent loss includes procedures in which lesions are long, calcified or tortuous. The stent is captured within the lesion and only balloon escapes (stent entrapment), the proximal part of the stent is deformed during insertion into the lesion and the stent is pulled during retraction within the guide catheter, and during the insertion of the stent into the lesion, the stent cannot pass and only the balloon passes (stent push-back). Four scenarios may then present to the operator [6] and recently tailored algorithms are suggested [7,8]:
• Partial stent loss in the coronary artery with the guide wire in situ
• Total stent loss in the coronary artery with the guide wire in situ
• Total stent and guide wire loss in the coronary artery
• Coronary stent loss in the aorta or peripheral circulation
Both cases were secondary to stent entrapment; in tortuous vessel for the first case, and in a long lesion for the second one. In the first case, that fits the second scenario an attempt to pass a small balloon into the stent and to inflate it slightly in order to retrieve the stent may be helpful. But wasn’t successful in our case we were committed to fix the stent. The second case fits the first scenario and a slight inflation of the stent’s balloon was sufficient to retrieve the stent.
Literature reviewing showed that in most cases stent could be retrieved and if not possible it could be fixed in the complication site [9,10]. Outcomes are favorable in most cases; but serious complications (death, urgent coronary artery bypass graft and myocardial infarction) are related to CSL. In our series successful management could be achieved and outcomes were positive.
Conclusion
Stent loss is not an exceptional complication of PCI and could be life threatening. Management techniques are successful in the majority of cases and should be known by operators. Better coronary stenosis analysis and preparation for stenting may prevent this issue.
References
- Alomar ME, Michael TT, Patel VG, et al. Stent loss and retrieval during percutaneous coronary interventions: a systematic review and meta-analysis. J Invasive Cardiol. 25(12): 637–41 (2013).
- Shim BJ, Lee JM, Lee SJ, et al. ftree Cases of Non-Surgical Treatment of Stent Loss During Percutaneous Coronary Intervention. Korean Circ J. 40(10): 530-5 (2010).
- Kharge J, Sreekumar P, Swamy K, et al. Balloon-Assisted Retrieval of a Broken Stent-Delivery System. Tex Heart Inst J. 39(5): 644-6 (2012).
- Singh V, Khare R, Chandra S, et al. Dislodgement of a sirolimus- eluting stent in the right coronary artery and its successful deployment with a small-balloon technique. J Indian Coll Cardiol. 4(1): 44-6 (2014).
- Yasuda M, Spaccarotella C, Mongiardo A, et al. Migration of a stent from left main and its retrieval from femoral artery: A case report. Med. 96 (50): e9281 (2017).
- Complications: coronary stent loss [Internet].PCR Online. Available from:https://www.pcronline.com/Cases-resources-> images/Complications/Implant-loss/Stent-loss
- Partial stent loss: balloon partially on the stent [Internet]. PCR Online. Available from: https://www.pcronline.com/Cases-resources-images/Complications/Implant-loss/Stent-loss/partial- stent-loss
- Total stent loss with guidewire in situ [Internet]. PCR Online. Available from:https://www.pcronline.com/Cases-resources-images/Complications/Implant-loss/Stent-loss/Total-stent-loss/Total-stent-loss-GW-in-situ
- Iturbe JM, Abdel-Karim A-RR, Papayannis A, et al. Frequency, treatment, and consequences of device loss and entrapment in contemporary percutaneous coronary interventions. J Invasive Cardiol. 24(5): 215-21 (2012).
- Kammler J, Leisch F, Kerschner K, et al. Long-term follow- up in patients with lost coronary stents during interventional procedures. Am J Cardiol. 98(3): 367-9 (2006).