Research Article - Clinical Investigation (2017) Volume 7, Issue 1
The Practice and Safety of Injecting Insulin through Clothes among Patients with Diabetes in Bahrain
- Corresponding Author:
- Husain T
Department of Internal Medicine
Salmanyia Medical Xomplex (SMC), Bahrain
E-mail: husaintaha74@yahoo.com
Submitted: 08 February 2017; Accepted: 14 April 2017; Published online: 28 April 2017
Abstract
Background: The prevalence of diabetes mellitus has risen dramatically in the last two decades worldwide and it’s estimated to rise to 642 million in 2040.The prevalence rate of people with diabetic Mellitus in Kingdom of Bahrain is around 14.8% and that of type one diabetes is (3.4%) in 2007. Thousands of people are injecting insulin once or more than two times per day. Injecting insulin technique is vital to preserve correct dose, safety practice of administering insulin. Many people with diabetes have been observed to inject their insulin through clothes for long time and many of the antiseptic techniques which are recommended by the health care professionals are challenged to be unnecessary. Aim: To improve the practice of injecting insulin among diabetes mellitus patients. Objective: To identify possible factors associated with the practice of injecting insulin through clothes amongst patients with diabetes and its safety. Methods: A Cross sectional study. Sample size and sampling technique: The data were collected from 100 diabetic patients who were on insulin therapy in Bahrain. Self-administered questionnaire was formulated for data collection. It contained: demographic data, the practice of injecting insulin through clothes, the possible factors associated with injecting insulin through cloths, and its related complications. Results: Seventy-four (74%) of the subjects were females. Thirty (30%) participants are 20 years old or below. Thirty (30%) participants are injecting insulin through clothes. It was complicated by erythema in (9%), minor bleeding (3%), cellulitis (2%) and Pus (1%). Eight subjects (8%) needed medical treatment and one subject (1%) required surgical intervention for the complication. (17%) of the subjects were using this technique during emergency situations, (12%) of the subjects used it due to embarrassment. Experiencing high blood sugar after injecting through clothes was experienced in (7%) of the subjects. Conclusion: Injecting insulin through clothes is not unusual practice among patients with diabetes which is associated with complications.
Keywords
Diabetic mellitus, Insulin injection, Injecting insulin technique, Safety, Clothing
Introduction
Diabetes is becoming a major growing medical problem worldwide. It is a chronic progressive metabolic disease characterizes by high levels of blood sugar. It’s caused by a defect in insulin production by the pancreas or due to tissue insulin resistance or both. Diabetes is one of the most important causes of blindness, kidney failure, cardiovascular disease, limb amputation and death. Diabetes prevalence has doubled since 1980. It has risen from 4.7% in 1980 to 8.5% in 2014 with the Eastern Mediterranean region having the highest prevalence 13.7 % [1]. In 2015, the estimated number of people with diabetes worldwide is 415 million and it’s estimated to rise to 642 million in 2040 [2]. In the Middle East and North Africa (MENA) region, the prevalence of diabetes is estimated to be 35.4 million people (9.1% of adults aged 20-79) over 40.6% of these are undiagnosed. This prevalence expected to rise to 11.4% in the MINA region by 2040 [2]. In our Country, Bahrain, one of the countries of MENA region, the prevalence of diabetes is 14.3% (253 cases) in the age group 20-64 years in 2007 [3]. Bahrain is reported by the IDF to be the third in MENA region after Saudi Arabia and Kuwait in the prevalence of Diabetes in 2014. In 2015, the IDF reported data about diabetes in Bahrain: 154,300 million adults with diabetes, with 800 adults with diabetes related deaths [4]. Diabetes and its complications are causing a growing burden on the individual, their family and their society. It has a high burden on the health cost and on wellbeing and mortality. In 2015, Diabetes caused 5 million deaths, which is the highest compared to mortality caused by HIV, TB, and malaria: 1.5, 1.5, and 0.6 million respectively [2].
Teaching patients the proper injecting insulin technique is vital for health care professionals to preserve correct dose, safety practice of administering insulin. Insulin injection emphasized sterilization technique previously [5], however the antiseptic utility of quickly swabbing the site of insulin injection with alcohol has been refuted [6,7]. The ADA statement on insulin administration neither directly advocates nor condemns the use of alcohol swabs, but it recommends that if it’s used the patient should wait till it evaporates before injection of insulin [8]. Cellulites, inflammation and other local complications among diabetes patients can occur. Health care providers should examine the sites of insulin injecting during their clinic visits. Patients should also be advised to rotate the injection sites to prevent the local complications [8]. Sometimes when the patients outside in public or at work were its difficult to find a private place to unclothe and inject the insulin, they will inject insulin through their clothes in which they found it more convenient, more time saving and less embarrassing. In 1997, Fleming et al provide convincing evidence that injecting insulin through clothing is more convenient and shows no higher risk of skin infection or skin reactions, so removing an important barrier to attain diabetic control [9].
This study will identify the possible causes that lead to practice of injecting insulin through clothes and the related complications that patients with diabetes and if this way of injecting insulin is safe.
Methods
Study design
Cross sectional study.
Data collection tool
Self-administered questionnaire was formulated for data collection. It contained: demographic data, the practice of injecting insulin through clothes, the possible factors associated with injecting insulin through cloths, and its related complications.
Data collection
Data collection was done during the period from June 21; through July 30th 2016. Patient identity was kept confidential at all times. The questionnaire distributed to the participants was formed by the survey monkey.
Ethical consideration
Patients were not placed at any risk by the study; therapy decisions were not based on the study, and no financial compensation was offered for participation. Ethics committee approval was nevertheless obtained.
Results
Table 1 is showing the demographic characteristics of the participants. Overall, 74% were females. Thirty percent were 20 years old or less and 24% were 53 years old or more. The vast majority of participants’ never injected insulin through clothing, only 30% had injected insulin through clothing where 18% of them were practicing that at least once per week and 15% of them were practicing that at least once per month. Twenty eight percent of them didn’t experience any complications.
| Characteristic | Patients (NO.) | Patients (%) | |
|---|---|---|---|
| Sex | Male | 26 | 26 |
| Female | 74 | 74 | |
| Age (years) | 20 or below | 30 | 30 |
| 21-31 | 19 | 19 | |
| 32-42 | 12 | 12 | |
| 43-53 | 15 | 15 | |
| 54 or more | 24 | 24 | |
Table 1: The demographic data of the study participants
Table 2 is showing the frequency of associated complications in participants who were practicing injecting insulin through clothing. Erythema was the most encountered complication 9%, followed by bleeding 3%, cellulitis 2% and pus 1%. Therapeutic intervention was needed in 8 % of those who experienced complications. Therapeutic interventions were in the form of local ointments or creams in 15%, systemic antibiotics in 4%, surgical drainage in 1%.
| Observed complications | Patients (%) | |
|---|---|---|
| Complications locally at site of injecting through clothes | erythema | 9 |
| bleeding | 3 | |
| cellulitis | 2 | |
| Pus | 1 | |
| Injecting technique problems | needle kinked | 7 |
| needle not penetrating the clothes | 6 | |
| glycemic control | hyperglycemia | 7 |
Table 2: Percentage of complications among patients injecting insulin through clothing
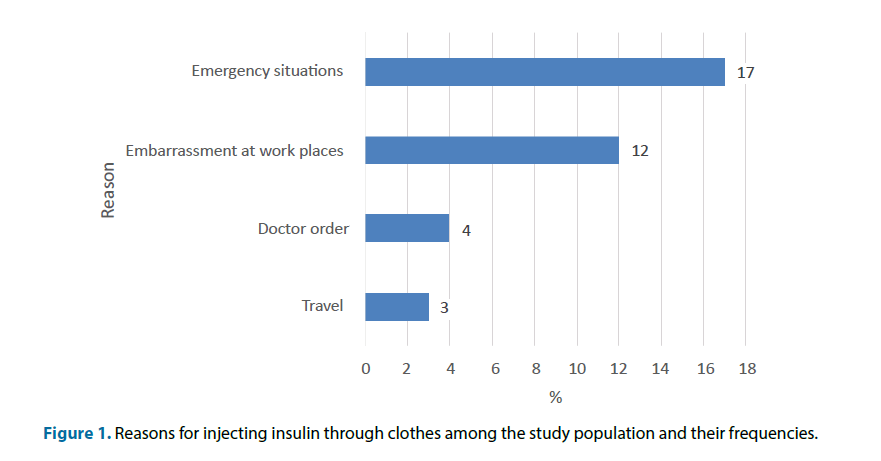
Figure 1 is showing the reasons which was reported by the participants behind their practice of injecting through clothing. Majority of them reported that they were in emergency situations (17%) or feeling embarrassed at work places (12%).
Discussion and Conclusion
In our study, the percentage of patients with diabetes practicing injecting insulin through clothing was 30% from the participants while the majorities were not. The Insulin Injection Questionnaire (ITQ) survey was conducted among 13,289 patients from 42 countries worldwide which were about the injecting practice of insulin from February, 2014 until June, 2015. ITQ survey revealed only 8% of the enrolled patient’s injected insulin through clothing, which is, much less than the percentage from our study in Bahrain [9]. Furthermore, the majority (28%) of those injecting insulin through clothing, didn’t develop any difficulty in injecting technique, local complications or hyperglycemia. Our data showed that erythema is the most frequent encountered local injection site complication if insulin is injected through clothing which was reported by 9% of the participants. On the other hand, pus was the least encountered one which occurred in only 1%. Only 1% needed surgical intervention while the remaining needed local ointments (15%), systemic antibiotics (4%). However, a single- blinded prospective study conducted in America in 1994-1995 about the safety of injecting insulin through clothing revealed that none of the enrolled subjects experienced erythema, induration or abscess at injection sites nor changes in glycemic control, but only bruises and blood stains on clothing were reported during the injection-through-clothing phase of the study [9]. Furthermore, our research explored the reasons behind injecting insulin through clothing, including traveling, following doctor order or feeling embarrassed in work places and these account for 3%, 4% and 12% respectively. These reasons were almost similar to those in a study published in America, where it was determined by the open-ended comments that subjects found that injection though-clothing technique convenient especially when they are away from home, particularly at work and in restaurants [9]. The importance of skin disinfecting before insulin injection has been disputed for many years ago. Since most insulin preparation has bacteriostatic additives which inhibit the growth of any bacteria and insulin injection is primary done at home not in hospitals where virulent organisms are not common. Current guidelines for insulin injection do not make reference to injecting insulin through clothing as an option [9].
The practice of insulin injection-through clothing is not uncommon among patients with diabetes followed up in the hospital. Patients with diabetes are hampered by injection of insulin and exposing their bodies outside their homes and in public. It is a fast technique and convenient for the patients in special situations, however it’s difficult to judge the safety of Insulin injecting through clothing by only our study’s results. There are some limitations in our study. The number of population involved is small.
Scanty studies worldwide and no studies in the Middle East region have been done regarding injecting insulin through clothing. Further studies are warranted locally and worldwide to identify the factors associated with the safety of injection of insulin through clothing.
References
- WHO (2016) Global report on diabetes. Available at: http://www.who.int/diabetes/global-report/en/ (Accessed: 29 January 2017).
- IDF diabetes atlas - Home [Internet]. Diabetesatlas.org. 2016.
- National non communicable disease risk factor survey. Ministry of Health, Bahrain. 2007.
- IDF diabetes atlas. The country report (Bahrain). 2015.
- Diabetic care in pictures: Simplified statements with illustrations prepared for the use of the patient. Journal of the American Medical Association, 133(11), p. 807 (1947).
- Fleming DR. ‘Challenging traditional insulin injection practices’. American Journal of Nursing, 99(2): 72–74 (1999).
- Rathod M, Saravolatz L, Pohlod D, Whitehouse F and Goldman J. ‘Evaluation of the sterility and stability of insulin from Multidose Vials used for prolonged periods’. Infection Control, 6(12): 491–494 (1985).
- American Diabetes Association. Insulin administration. Diabetes Care, 19(1): 31–34 (1996).
- Fleming DR, Jacober SJ, Vandenberg MA, Fitzgerald JT, Grunberger G. ‘The safety of injecting insulin through clothing’. Diabetes Care, 20(3): 244–247 (1997).