Case Report - Research on Chronic Diseases (2017) Volume 1, Issue 1
Serotonin syndrome masked by fibromyalgia: a case report
- *Corresponding Author:
- Ference T
Miller School of Medicine
University of Miami, USA
E-mail: t.ference@med.miami.edu
Abstract
Fibromyalgia is a disorder characterized by widespread myalgia, fatigue, and hyperesthesia. It also may present with mood fluctuation, insomnia, and memory issues. It has 1.75% prevalence in the US, affecting approximately 3.94 million persons. Although the full pathophysiology is still unknown, it is widely believed to be secondary to a lower pain threshold in the central nervous system, termed “central sensitization”. This hyperactivity can be attenuated by activating the pain modulatory circuit of the CNS3. Selective Serotonin Reuptake Inhibitors (SSRIs) are most likely active in this circuit, and have proven efficacy as adjunct therapy in management of pain due to fibromyalgia. This effect is independent of its antidepressant activity, so use of these drugs is not limited to patients with fibromyalgia and depression.
Keywords
pathology, clinical pathology
Introduction
Fibromyalgia is a disorder characterized by widespread myalgia, fatigue, and hyperesthesia. It also may present with mood fluctuation, insomnia, and memory issues. It has 1.75% prevalence in the US, affecting approximately 3.94 million persons [1]. Although the full pathophysiology is still unknown, it is widely believed to be secondary to a lower pain threshold in the central nervous system, termed “central sensitization” [2]. This hyperactivity can be attenuated by activating the pain modulatory circuit of the CNS3. Selective Serotonin Reuptake Inhibitors (SSRIs) are most likely active in this circuit [3], and have proven efficacy as adjunct therapy in management of pain due to fibromyalgia [4]. This effect is independent of its antidepressant activity [5], so use of these drugs is not limited to patients with fibromyalgia and depression.
Although SSRIs generally have a favourable side effect profile, the most feared complication of these drugs is serotonin syndrome. Interactions with other serotonin promoting drugs is the most common cause of serotonin syndrome [6]. Patients with fibromyalgia are typically taking a myriad of medications. Additionally, features of fibromyalgia may mask features of serotonin syndrome. It is important that physicians are aware of this overlap when managing patients with chronic pain.
Case description
A 56-year-old female with a past medical history of hypertension, asthma, and fibromyalgia presented to clinic for management of her fibromyalgia. The patient was well known to the clinic. The course of her syndrome was characterized by a stable medication regimen that included milnacipran, zolpidem, pregabalin, and vitamin supplementation (vitamin B complex daily, vitamin C 500 mg daily). The patient’s fibromyalgia had been relatively well-controlled throughout her ten-year course. However, her symptoms upon presentation to clinic were different than her baseline. She complained of hot flashes, intermittent headaches, and an increase in her generalized pain.
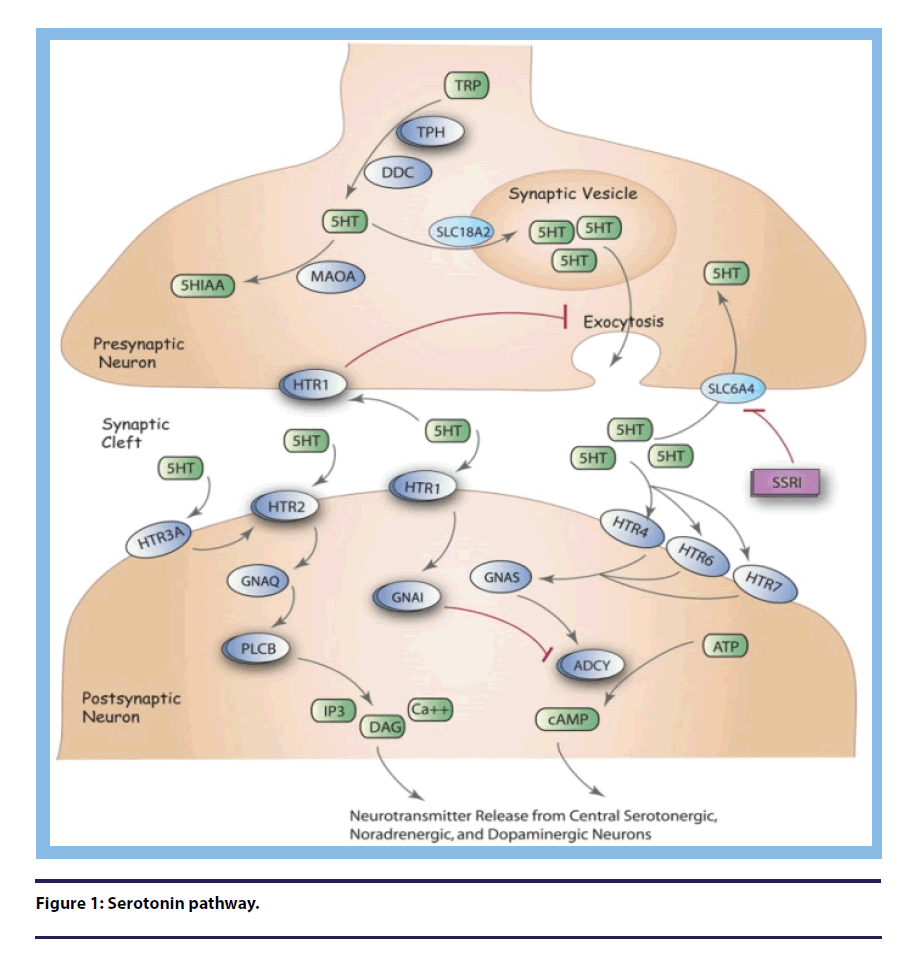
On further interrogation of the patient history, it was revealed that her primary care physician started her on tramadol. The physical exam revealed a tachycardic patient with flushed skin. She did not have any long tract signs, hyperthermia, dilated pupils, or clonus, but she was noted to be mildly agitated and easy to fatigue (Figure 1).
Figure 1: Serotonin pathway.
Discussion
When a patient with fibromyalgia presents with symptoms that have changed from their baseline, it is important to perform a thorough history and physical exam to exclude other systemic problems that can mimic fibromyalgia. Patients are commonly placed on multiple medications to account for their pain, cognitive, and psychiatric disturbances [7]. This puts them at risk for unwanted drug interactions that make it difficult to differentiate a fibromyalgia exacerbation from a true serotonin syndrome. Serotonin syndrome is caused by increased level of serotonin in the CNS primarily via stimulation of the 5-HT receptor [8,9]. This can occur with an overdose of a single serotonergic medication or with two drugs working synergistically to release serotonin. The presenting symptoms of serotonin syndrome can vary from mild to severe. Mild to moderate signs and symptoms include tachycardia, diaphoresis, myoclonus, hypertension and hyperthermia [10]. In more severe cases, patients may present with shock, seizures, renal failure or metabolic acidosis [11]. One must maintain a high level of clinical suspicion for serotonin syndrome in a patient with atypical signs of fibromyalgia.
Conclusion
Serotonin syndrome is an acute life-threatening illness most commonly caused by polypharmacy. It is crucial to thoroughly evaluate a patient with chronic fibromyalgia whose symptoms have changed from their baseline. This case displays the overlap between symptoms of fibromyalgia and those of serotonin syndrome. All patients presenting with fibromyalgia warrant a thorough review of all their medications. One should have a high clinical suspicion of serotonin syndrome in these patients, especially when heavily medicated.
References
- Walitt B, Nahin RL, Katz RS et al. The prevalence and characteristics of fibromyalgia in the 2012 National health interview survey. PLoS ONE. 10(9), e0138024 (2015).
- Clauw DJ. Fibromyalgia: a clinical review. JAMA. 311(15), 1547–1555 (2014).
- Ossipov MH, Dussor GO, Porreca F. Central modulation of pain. J. Clin. Invest. 120(11), 3779–3787 (2015).
- Goldenberg DL, Mayskly M, Mossey C et al. A randomized, double–blind crossover trial of fluoxetine and amitriptyline in the treatment of fibromyalgia. Arthritis Rheum. 39(11), 1852–1859 (1999).
- Uher R, Maier W, Hauser J et al. Differential efficacy of escitalopram and nortriptyline on dimensional measures of depression. Br. J. Psychiatry. 194, 252–259 (2009).
- Watson WA, Litovitz TL, Rodgers GC et al. 2004 annual report of the American Association of Poison Control Centers Toxic Exposure Surveillance System. Am. J. Emerg. Med. 23, 589–666 (2005).
- Turner EH, Loftis JM, Blackwell AD. Serotonin a la carte: supplementation with the serotonin precursor 5–hydroxytryptophan. Pharmacol. Ther. 109, 325–338 (2006).
- Egberts AC, ter Borgh J, Brodie–Meijer CC. Serotonin syndrome attributed to tramadol addition to paroxetine therapy. Int. Clin. Psychopharmacol. 12, 181–182 (1997).
- Lane R, Baldwin D. Selective serotonin reuptake inhibitor–induced serotonin syndrome: review. J. Clin. Psychopharmacol. 17, 208–221 (1997).
- Sclar DA, Robison LM, Skaer TL. Concomitant triptan and SSRI or SNRI use: a risk for serotonin syndrome. Headache. 48, 126–129 (2008).
- Lavery S, Ravi H, McDaniel WW et al. Linezolid and serotonin syndrome. Psychosomatics. 42, 432–434 (2001).