Case Report - International Journal of Clinical Rheumatology (2017) Volume 12, Issue 4
Rituximab can induce remission in a patient with rheumatoid arthritis and Ankylosing spondylitis
- Corresponding Author:
- Betul Sargın
Physical Medicine and Rehabilitation Department
Rheumatology Division, Adnan Menderes University
Aydin, Turkey
E-mail: Arina.Bingeliene@uhn.ca
Abstract
The efficacy of Rituximab (RTX) has been examined in Ankylosing Spondylitis (AS) and Rheumatoid Arthritis (RA) before. Here, we have reported the case of a patient with RA and AS showing good clinical improvement with RTX. A 47-year-old female patient being followed by RA diagnosis presented with bilateral wrist pain and swelling for three months. Previously, she had received multiple DMARDs with poor response. For her ongoing active disease, Disease Activity Score 28 (DAS28=7.3) RTX 1000 mg was administered at 0 and second weeks. She had chronic inflammatory lower back pain with morning stiffness, which improved on exercise and hot shower since last two years. Suprapubic pelvis Anterior Posterior (AP) radiography and sacroiliac Magnetic Resonance Imaging (MRI) showed bilateral sacroiliitis. She was diagnosed as AS and showed significant response to RTX. DAS28, ASDAS and BASDAI scores reduced. CRP level was decreased significantly. Concomitant AS and RA patients should be carefully followed and RTX treatment should be kept in mind in these patients.
Keywords
rituximab, rheumatoid arthritis, spondylitis, ankylosing
Introduction
Rheumatoid Arthritis (RA) is a chronic autoimmune disease characterized by progressive articular disability, systemic inflammation and high morbidity [1]. Multiple cell types play a role in the pathogenesis of RA, the key participation is B cells [2]. Ankylosing Spondylitis (AS) is a chronic inflammatory disease that predominantly affects the axial skeleton [3]. CD3+, CD4+, CD8+ T and CD20+ B cells were found in the Sacroiliac (SI) joints of patients with AS [4]. As a result, B cells play a key role in the pathogenesis of RA and AS. Rituximab (RTX) is a chimeric monoclonal anti-CD20 antibody that induces depletion of peripheral CD20-positive B cells [5]. Here, we have reported the case of a patient with RA and AS showing good clinical improvement with RTX.
Case presentation
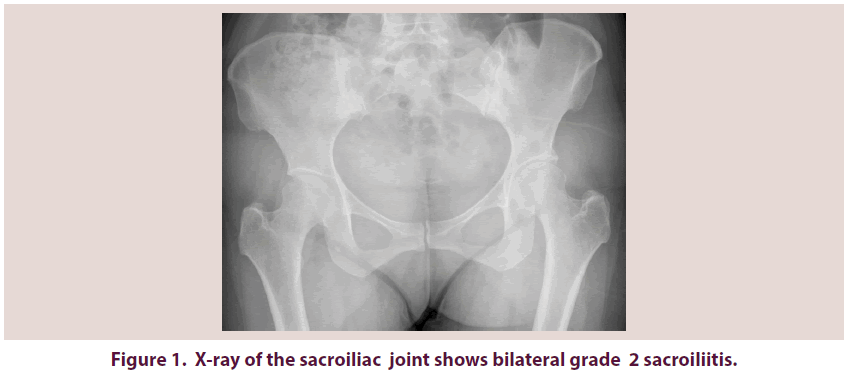
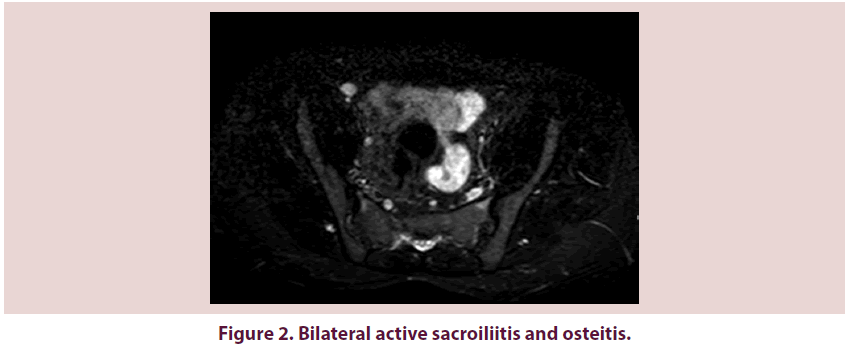
A 47-year-old female patient being followed by RA diagnosis presented to the rheumatology clinic, Adnan Menderes University with bilateral wrist pain and swelling for three months. Previously, she had received multiple DMARDs (MTX, sulfasalazine and hydroxychloroquine) with poor response. For her ongoing active disease, Disease Activity Score 28 (DAS28=7.3) RTX 1000 mg was administered at 0 and second weeks. She had chronic inflammatory lower back pain with morning stiffness, which improved on exercise and hot shower since last two years. She had received meloxicam 15 mg for her lower back pain. She was admitted to our rheumatology clinic for these reasons. A written informed consent was obtained from the patient. The general condition was moderate, oriented and cooperated. Locomotor system examination revealed tenderness and painful of the both wrists. She had marked limitation of spinal movement, chest expansion was 3 cm, modified Schober test was 2 cm, finger to floor distance was 23 cm, tragus wall distance was 11 cm, lumbar lateral flexion distance was 9 cm, and intermalleolar distance was 62 cm. The other system examinations were normal. Ankylosing Spondylitis Disease Activity Score (ASDAS) was 4.6, Bath Ankylosing Spondylitis Disease Activity Index (BASDAI) was 5.7, C-Reactive Protein (CRP) was 39.00 mg/dL. Suprapubic pelvis Anterior Posterior (AP) radiography showed bilateral grade 2 sacroiliitis (Figure 1) and sacroiliac Magnetic Resonance Imaging (MRI) showed bilateral active sacroiliitis and osteitis (Figure 2). According to these findings she was diagnosed as AS. Response to treatment was assessed by DAS28, ASDAS, BASDAI scores, CRP levels and spinal measurements. She showed significant improvement clinically; chest expansion was 5 cm, modified Schober test was 6 cm, finger to floor distance was 10 cm, tragus wall distance was 9, lumbar lateral flexion distance was 11 cm, intermalleolar distance was 71 cm. DAS28, ASDAS and BASDAI scores reduced to 2.1, 1.3 and 3.00, respectively. CRP level was 3 mg/dL after treatment. Figure 3 shows the clinical and biochemical response to RTX treatment.
Discussion and conclusion
This case report describes a good response to RTX in a patient who was diagnosed as RA and AS. The patient showed significant response to RTX. DAS28, ASDAS and BASDAI scores reduced from 7.3 to 2.1, 4.6 to 1.3 and from 5.7 to 3.00, respectively. Also, CRP level was decreased significantly from 39 mg\dL to 3 mg\dL (Figure 3).The key participation in the pathogenesis of RA is B cells [2]. CD3+, CD4+, CD8+ T and CD20+ B cells were found in the SI joints of patients with AS [4]. RTX is a chimeric monoclonal anti-CD20 antibody that induces depletion of peripheral CD20-positive B cells. It was approved for use in patients with RA in 2006 [5]. The efficacy of RTX has been examined in AS [3,6-12] and RA before. It was found to be efficacious in RA patients, including those who are MTX naive, those with an incomplete response to MTX, and those with an incomplete response to tumor necrosis factor inhibitors (TNFI) [13]. It is administered intravenously with a total dose of 1000 mg at 0 and second weeks. Intravenous corticosteroid is used for premedication [14]. Rodríguez et al. [6] reported the first case report of RTX treatment in a patient with AS and hepatitis B. In 2011, Huang et al. [7] evaluated the first description of improvement of active inflammation on MRI after RTX administration in a patient with active AS. Omair et al. [8] presented a case of AS who developed demyelinating disease secondary to TNFI and was treated successfully with RTX. Dundar et al. [9] reported the first case of successful RTX treatment in a patient with RA and AS. Song et al. [10] phase II clinical trial investigated RTX treatment in 20 patients with active AS. Ten of these patients had never received TNF blockers, the others had failed with TNF blockers. In the TNF blocker-naive group a good improvement was received at week 24. Kiltz et al. [11] analyzed the treatment of AS patient’s refractory to TNFI. As a result of their study data for abatacept, anakinra, apremilast, bisphosphonates, RTX, secukinumab, sulfasalazine, thalidomide and tocilizumab were found. But none of these new drugs has been shown to reach response rates compared to TNF-blockers. Wendling et al. [12] evaluated the efficacy and safety of RTX in a total of 26 patients with Spondyloarthritis (SpA) [10] (AS), 7 undifferentiated SpA, and 9 Psoriatic Arthritis (PsA)]. Efficacy of RTX was noted in 11 cases: 3 were anti-TNF-naive patients and 8 were anti- TNF nonresponder patients. As a result of their study RTX had moderate efficacy in patients who were anti-TNF-naive.
Our case report is the second case of successful RTX treatment in a patient with RA and AS. We suggest that B cell directed therapies are a newly identified trend in concomitant AS and RA patients. Concomitant AS and RA patients should be carefully followed and RTX treatment should be kept in mind in these patients, the patients should be examined in this respect.
References
- Smolen JS, Aletaha D, McInnes IB. Rheumatoid arthritis. Lancet. 388(10055), 2023–2038 (2016).
- Adlowitz DG, Barnard J, Biear JN et al. expansion of activated peripheral blood memory B cells in rheumatoid arthritis, impact of B cell depletion therapy, and biomarkers of response. PloS ONE. 10(6), e0128269 (2015).
- AlDhaheri F, Almteri T, Dwid N et al. Rituximab can induce remission in a patient with ankylosing spondylitis who failed anti-TNF-α agent. Am. J. Case. Rep. 18, 143–147 (2017).
- Braun J, Bollow M, Neure L et al. Use of immunohistologic and in situ hybridization techniques in the examination of sacroiliac joint biopsy specimens from patients with ankylosing spondylitis. Arthritis Rheum. 38(4), 499–505 (1995).
- Schmalzing M, Tony HP. B cell therapy of rheumatoid arthritis with rituximab. Practice-relevant aspects for the routine. Z. Rheumatol. 74(3), 250–257 (2015).
- Rodríguez-Escalera C, Fernández-Nebro A. The use of rituximab to treat a patient with ankylosing spondylitis and hepatitis B. Rheumatology (Oxford). 47(11), 1732–1733 (2008).
- Huang Y, Cheng F, Zhang X et al. Marked reduction of sacroiliac joint inflammation on magnetic resonance imaging in a patient with ankylosing spondylitis after rituximab treatment. J. Rheumatol. 38(9), 2083–2084 (2011).
- Omair MA, Alnaqbi KA, Lee P. Rituximab in a patient with ankylosing spondylitis with demyelinating disease: a case report and review of the literature. Clin. Rheumatol. 31(8), 1259–1261 (2012).
- Dundar U, Çevik H, Demirdal US et al. Use of rituximab to treat a patient with coexistence of rheumatoid arthritis and ankylosing spondylitis: 18 months follow-up. Int. J. Rheum. Dis. (2014).
- Song IH, Heldmann F, Rudwaleit M et al. Different response to rituximab in tumor necrosis factor blocker-naive patients with active ankylosing spondylitis and in patients in whom tumor necrosis factor blockers have failed: a twenty–four-week clinical trial. Arthritis Rheum. 62(5), 1290–1297 (2010).
- Kiltz U, Heldmann F, Baraliakos X et al. Treatment of ankylosing spondylitis in patients refractory to TNF-inhibition: are there alternatives? Curr. Opin. Rheumatol. 24(3), 252–260 (2012).
- Wendling D, Dougados M, Berenbaum F et al. Rituximab treatment for spondyloarthritis. A nationwide series: data from the AIR registry of the French Society of Rheumatology. J. Rheumatol. 39(12), 2327–2331 (2012).
- Cohen MD, Keystone E. Rituximab for rheumatoid arthritis. Rheumatol. Ther. 2(2), 99–111 (2015).
- Buch MH, Smolen JS, Betteridge N et al. Updated consensus statement on the use of rituximab in patients with rheumatoid arthritis. Ann. Rheum. Dis. 70(6), 909–920 (2011).